High Risk Pregnancy
What is a High Risk Pregnancy?
A high risk pregnancy is one that involves a significant health risk to the baby or the expectant mother or both. High risk pregnancies require close prenatal monitoring, testing, and care to lower the chance of birth complications and birth injury. Timely diagnosis of the risks during pregnancy, labor and delivery, and proper management can help protect the health of the baby and the mother.

According to the American Pregnancy Association, doctors like obstetricians and maternal fetal medicine specialists should plan for more frequent prenatal visits in case of a high-risk pregnancy in order to better monitor the baby’s development. Birth complications like premature birth, miscarriage, birth defects, and birth injuries such as hypoxic-ischemic encephalopathy (which can lead to cerebral palsy) may occur if a high-risk pregnancy is mismanaged or not diagnosed on time. This may constitute medical negligence if the resulting birth injury was preventable.
When a woman is determined to be a high risk pregnancy, there are certain obstetrician physicians that have additional training in handling these type of pregnancies called maternal-fetal specialists. Whenever an expectant mother is deemed high risk, the best course is for her obstetrician to involve a maternal-fetal specialist in her prenatal care and labor and delivery.
How is a High Risk Pregnancy and HIE related?
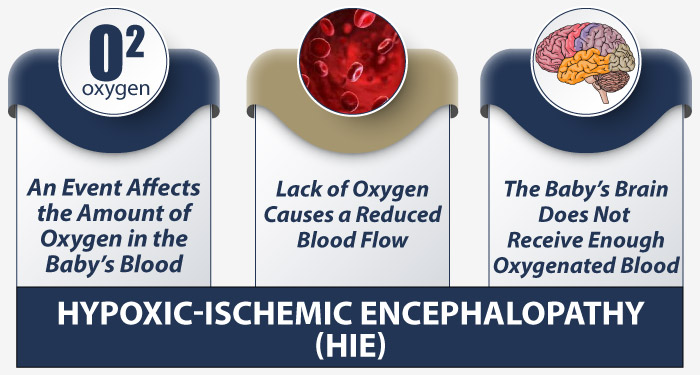
High risk pregnancies have an increased correlation with hypoxic-ischemic encephalopathy (HIE) because a variety of birth complications may arise during labor and delivery, which could severely reduce oxygen supply to the baby’s brain. This can cause brain damage, and eventually lead to cerebral palsy. To minimize the risk of HIE, the medical provider should conduct more frequent prenatal tests to identify if the baby is experienced fetal distress.
These tests may include fetal ultrasounds, fetal heart rate monitoring, non-stress tests (NSTs), and biophysical profile (BPP) tests. If the medical provider suspects birth complications, such as HIE or other serious birth injury risks, they should be prepared ahead of time to perform a cesarean section if necessary. The medical team should also be ready to perform neonatal resuscitation and neuroprotective procedures such as hypothermia therapy in a timely and correct manner when required at birth.
What are the Risk Factors for a High Risk Pregnancy?
The medical provider should be vigilant to the following risk factors that may indicate a high-risk pregnancy:
- Pregnancy Complications: Unusual position of the placenta like placenta previa, intrauterine growth restriction (fetal growth is restricted for its gestational age), umbilical cord prolapse, and Rh sensitization (mother’s blood is Rh negative and the developing baby is Rh positive) are some of the examples of complications during pregnancy, which can pose risks.
- Maternal Health Conditions: Gestational diabetes, maternal hypertension (preeclampsia), maternal infections such as Group B Strep, thyroid disease, asthma, obesity, epilepsy, blood disorders, kidney disease, PCOS (polycystic ovary syndrome), fibroids, or cardiovascular disease may increase the risks during pregnancy.
- Pregnancy History: A history of miscarriage, stillbirth, premature birth, premature rupture of membranes (PROM), multiple births, pregnancy related high blood pressure or gestational diabetes in a previous pregnancy can increase the risks of the next pregnancy.
- Other Risk Factors: Advanced maternal age (especially if the mother is above 35 years of age), multiple pregnancy (carrying twins, triplets or other multiples), and lifestyle choices, such as drinking alcohol, smoking or substance abuse during pregnancy may contribute to a high risk pregnancy.
- High Blood Pressure and Preeclampsia: These related conditions can lead to serious birth complications for both the expectant mother and her baby. Doctors must monitor these high risk pregnancies for birth complications such as preeclampsia, HELLP syndrome and placental abruption.
- Previous Caesarean: If a vaginal delivery is going to be attempted. This is commonly referred to as a vaginal birth after caesarean (VBAC).
Visible Signs and Symptoms
While prenatal testing, fetal monitoring, medical tests and a review of medical history are important ways to diagnose a high risk pregnancy, some of the visible signs and symptoms should also alert the medical provider to the possibility of a high risk pregnancy. These include:
- Persistent abdominal pain
- Fainting or dizziness
- Chest discomfort or tightness
- Excessive fatigue
- Slowing down of the fetal movement
- Heart palpitations
- Breathing difficulties
- Fever above 100.4° F
- Vomiting and nausea, which becomes unusually worse than morning sickness
- Pain, redness or swelling in the limbs or face
- Severe headache that does not resolve or worsens
- Vaginal discharge or bleeding
How Should Labor and Delivery be Managed in a High Risk Pregnancy?
Ultrasound Examination
More frequent ultrasound scans must be performed at multiple stages during a high risk pregnancy for the following reasons:
- First Trimester
- To identify multiple babies
- To examine the pelvic anatomy, and in particular the uterus
- To detect birth defects
- To diagnose a miscarriage
- Second Trimester
- To examine the baby for birth abnormalities
- To evaluate blood flow patterns
- To find any serious dysfunction in the umbilical cord
- To measure the length of the cervix length
- The measure the amniotic fluid volume
- To observe any abnormal changes in fetal activity
- To monitor the baby’s growth
- Third Trimester
- To perform the BPP test (biophysical profile)
- To monitor fetal growth
- To measure the amniotic fluid volume
- To determine the baby’s position
- To look for potential placental abnormalities and determine the risk of premature delivery, intrauterine growth restriction (IUGR), and brain damage.
Non-Stress Tests (NST)
A non-stress test (NST) is generally performed from 38 to 42 weeks, but in case of high-risk pregnancy it should be performed earlier. The test will indicate how the baby’s heart rate functions in response to movement. If the heart rate is slow, the medical provider should be alert to the possibility of oxygen deprivation (fetal hypoxia), which is a risk factor for hypoxic-ischemic encephalopathy (potentially leading to cerebral palsy). An emergency cesarean section may have to be planned along with preparations for hypothermia therapy.
Biophysical Profile (BPP) Test
In a high risk pregnancy, the biophysical profile (BPP) test should be performed in the second trimester (it is usually performed in the third trimester for normal pregnancies). In the third trimester, considering the high-risk pregnancy, the medical provider should recommend a BPP test to be undertaken once or twice a week or even more frequently in some cases. The BPP test includes ultrasound exams, non-stress tests, amniotic fluid measurement, and fetal heart rate monitoring to identify risks, such as hypoxic-ischemic encephalopathy (HIE), and fetal acidosis.
Delayed Cesarean Section
When the risks of a vaginal delivery outweigh the benefits in a high risk pregnancy, the medical provider should be prepared to perform a planned or emergency cesarean section. In many high risk situations, just a few minutes of delay in performing an emergency c-section can result in serious or permanent birth injuries. If the cesarean section is delayed or labor is prolonged beyond a safe limit, it may cause oxygen deprivation to the baby, resulting in HIE and potentially leading to cerebral palsy.
Vacuum Extraction or Forceps Injuries
A high risk pregnancy may lead to a situation where the medical team decides to perform an assisted vaginal delivery, using vacuum extractors or forceps. They will use these devices to enable the baby to move down the birth canal if the vaginal birth is stalled or strained. Improper use of these devices or application of undue force can cause injuries to the baby and increase the risks of brain damage.
Improper or Irregular Fetal Monitoring
In a high risk pregnancy, the most effective way for medical providers to determine whether the baby is receiving adequate oxygen and to detect the signs of fetal distress is electronic fetal heart rate monitoring. If the baby’s heart rate is too low (bradycardia) or too high (tachycardia), or is otherwise fluctuating abnormally with recurrent late or variable decelerations, the medical provider should recognize these as signs of fetal distress and act fast to make appropriate interventions. Failure to monitor, improper monitoring, misinterpreting the fetal measurements, or failure to make appropriate medical interventions can increase the risks of birth injury or birth complication from a high-risk pregnancy.
Medication Errors
In high risk pregnancies that lead to prolonged or arrested labor, oxytocin (also called Pitocin) is a commonly used drug to induce or speed up labor. But an improper or excessive use of oxytocin can harm the baby by causing too long or too strong of contractions that lead to fetal distress. Researchers have described oxytocin and Pitocin as a “high-alert medication” and its appropriate initiation, measured usage, and timely discontinuation are critically important. Overuse or misuse of oxytocin, poor vigilance when oxytocin is administered intravenously, and lack of fetal monitoring during the labor induction process can result in serious birth injuries.
Is Your Child’s Birth Injury the Result of Medical Malpractice?
Parents whose children suffer birth injuries from a high risk pregnancy related birth trauma or birth complications want and deserve answers as to the cause of their child’s birth injury and whether mistakes by the doctors and nurses contributed to the injury.
- Were there signs of birth injury or birth complications during the pregnancy, labor, and delivery process, or presence of risk factors, which were either not recognized or properly treated?
- Was the pregnancy not handled as a high risk pregnancy despite clear signs and risk factors?
- During the labor and delivery, were there clear indications that the baby was suffering from fetal distress, but appropriate actions were not taken by the obstetrician or nurses?
- Was there a delay in diagnosis of a high risk pregnancy that led to later complications, including brain injury?
- Did the medical team fail to order a series of tests to diagnose this birth complication in a timely manner?
- Was the decision to perform a cesarean delivery delayed leading to birth trauma during vaginal delivery or labor?
- Did the neonatal resuscitation team fail to quickly begin important breathing support?
- Should brain cooling (also called “hypothermia therapy”) have been provided to your baby, but the doctors and nurses failed to perform the appropriate tests or ignored the results of the tests?
Our national birth injury attorneys have extensive experience in this and all areas of birth injury medical malpractice. The lawyers and nurses at Miller Weisbrod Olesky will help you determine if mistakes of the medical providers caused a birth injury to your child, including Hypoxic-Ischemic Encephalopathy (HIE) or cerebral palsy.
Our award-winning birth injury attorneys represent families all over the United States in their time of need after a wrongful birth. We use our skills and expertise to obtain for you and your child a medical malpractice settlement that will help provide specialized medical therapy in order to maximize the quality of life and independence of your child throughout their life.
Sometimes families are reluctant to contact a medical malpractice lawyer. It’s also not uncommon for parents to feel overwhelmed by the responsibilities they encounter in caring for their injured child and worried that they will not be able to help out in a lawsuit involving their child’s birth injury. Our birth injury attorneys and nursing staff will address these hesitations and concerns, so you can focus on your child and maximizing their care.
Registered Nurses and Nurse-Attorneys Are a Vital Part of Our Birth Injury Team…and Yours

Most birth injury law firms will employ one or two nurses to assist the review of cases and medical research. But Miller Weisbrod Olesky offers an unmatched number of nurses and nurse-attorney employees support to both the birth injury attorneys and our clients.
Our team of registered nursing staff and nurse-attorneys bring a deep level of medical and personal insight to every client’s case. Our nursing team includes both an experienced labor and delivery nurse as well as an ICU nurse. Working closely with the rest of the team, they investigate the reasons behind a birth injury and how medical professionals breached their standard of care.
Why Should You Talk with the Highly Capable Attorneys at Miller Weisbrod Olesky?

The only way to find out if you have a birth injury case is to talk to a lawyer experienced in birth injury lawsuits. It’s not uncommon that a birth related complication results in a preventable birth injury, including cerebral palsy, but it takes a detailed expert review by a birth injury attorney of the medical records from your child’s birth to determine if the birth injury was the result of medical malpractice.
At Miller Weisbrod Olesky, a team of committed lawyers, nurses and paralegals uses our detailed medical negligence case review process to assess your child’s potential birth injury case. We start by learning more about you and your child and the status of meeting/missing developmental milestones. Then we gather medical records to determine what happened before, during pregnancy. We call in documented and proven medical experts who review your records and let us know if they think medical errors could have caused your child’s injuries.
If we feel medical negligence caused or contributed to wrongful birth in your case, we meet with you to discuss how you can receive compensation from the medical professionals who made the errors. Our birth injury attorneys have recovered millions of dollars in settlements for families of children that have suffered a birth injury.
At no point in our legal intake process will we ask you to pay anything. The medical review of your case and the consultation are free. We only receive payment when you do no matter how long or tough your case is.
Contact Our Birth Injury Lawyers
National Birth Injury Law
Our National Birth Injury Attorneys, nurses, and support staff understand that parents of children with birth injuries feel overwhelmed. So, every client has the attention and support of a team of trained, compassionate professionals. But we don’t just offer compassion.
We offer a process to help you discover whether your child’s birth injury, HIE, cerebral palsy or brain injury at birth was caused by medical malpractice.
Call our offices today at (888) 987-0005 for experienced assistance in a free consultation.
Quick Links
Testimonials
- Lyric C. I feel like our voice was heard in a sense of what can possibly go wrong in a delivery and finding us answers. I feel with our settlement, we are now in a comfortable position to provide for our son.
- Lyssa L. They are not just people that say “hey let's get you money and let's go” The law firm was very thorough with us. It was awesome. I don't want to cry, because I think about and it's amazing that they were able to help me and that we were able to help my son and get the story out there.
- Jay C. Throughout the process, one thing was clear to us, the ultimate interest of our child was the utmost concern of Max and his team and as parents navigating a situation like that, that was refreshing to know we had them firmly on our side. I highly recommend them.
Popular Cities
- ★ Dallas Birth Injury
- ★ Houston Birth Injury
- ★ Atlanta Birth Injury
- ★ Chicago Birth Injury
- ★ Philadelphia Birth Injury
Locations
★ Dallas
11551 Forest Central Drive, Ste. 300
Dallas, TX 75243
★ Houston
12929 Gulf Freeway, Ste. 111
Houston, TX 77034