Maternal Infections
Maternal Infections During Pregnancy
Labor And Delivery Complications And Newborns
A mother’s body goes through incredible changes during pregnancy. The maternal immune system shifts to accommodate the fetus, suppressing certain hormonal and immunological processes so that her body does not reject the foreign entity that is the baby growing inside of her. These changes, however, make the expecting mother more susceptible to infections.
When uncaught or insufficiently treated, a maternal infection can make a mother extremely ill and even transfer to the baby in utero and progress into a dangerous neonatal infection. When a baby becomes infected, it can result in birth complications like prematurity and a low birth weight, or they can even serve as an underlying cause for a child’s sepsis or brain damage at birth.
It is the duty of OB-GYNs, nurses, midwives, and all other medical professionals to thoroughly screen an expecting mother during prenatal testing appointments for infections and any other pregnancy complications she may have. Most maternal infections are easily treatable with antibiotic or antiviral medications, but treatment is most effective when the infection is caught early.
Failing to catch or properly treat a maternal infection can lead to preventable birth defects and birth injuries for the child and constitute medical malpractice.
Over the past three decades, the nationally recognized team of birth injury attorneys at Miller Weisbrod Olesky has established a proven track record of delivering justice for children and families who have unfairly suffered from the consequences of birth injury negligence. Our firm is staffed with registered nurses and nurse attorneys to begin assisting your child with their treatment and therapy immediately.
We are prepared to meticulously investigate the circumstances of your case, gather crucial medical records, consult with top medical experts, and fight tirelessly to secure the compensation you deserve for your child’s injury, all at no upfront cost to you.
We represent families and their children in numerous service areas throughout the United States. You can contact us today to schedule your free legal consultation by calling our toll-free line at (888) 987-0005 or by filling out our online request form. We work on a contingency fee basis, meaning you won’t pay any legal fees, or costs unless we win your case. We only receive payment once you do.
What Causes Maternal Infections?
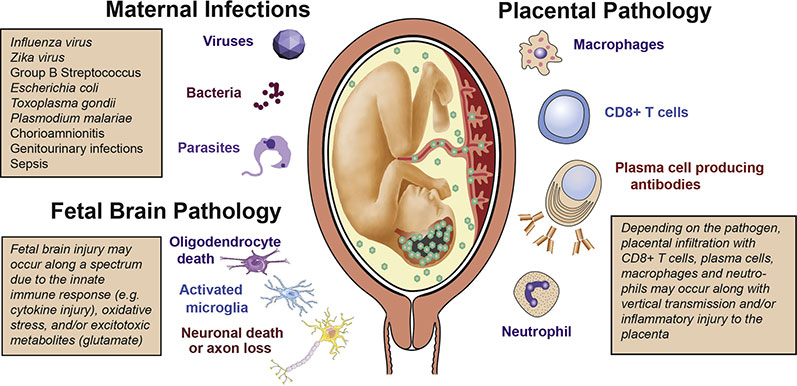
An infection is typically either bacterial or viral.
- Bacterial Infections: A bacterial infection occurs when foreign bacteria (microscopic living single-celled organisms) enter the mother’s body through some form of opening, whether on food and it’s ingested through the mouth, inhaled through breathing, or enters through contact with an open wound or cut.
The bacteria multiply and release toxins that can potentially damage surrounding cells and cause an inflammatory response. The most common maternal bacterial infections are Group B Streptococcus, bacterial vaginosis (BV) and urinary tract infections, as well as Escherichia Coli (E. Coli) and other food-borne pathogens. These types of infections are typically treated with antibiotic medications that kill the bacteria and prevent them from multiplying and spreading further.
It’s important to know that not all bacteria are bad; in fact, most of the human body is comprised of different bacteria that protect our immune systems. The bacteria discussed on this page are all classified as pathogenic, meaning they do not serve a helpful function and instead cause infection and disease. - Viral Infections: A virus is a small infectious agent that is only able to replicate (multiply) within the living cells of a “host” organism (humans or animals). A viral infection occurs when the virus successfully enters the body and begins to multiply within the cells.
A virus is technically not considered to be a living organism because it cannot reproduce independently. It must enter a host (in this case, the expecting mother) and hijack their cells. Common viral infections include influenza, COVID-19, Hepatitis B, and Herpes Simplex Virus. While some viral infections can be cured, others are not currently curable and can only be managed with medications.
Other types of infections include parasites, which work similarly to viruses but can also live outside of their host. The most common parasitic infection that expecting mothers are at risk for is toxoplasmosis.
What Are Common Maternal Infections?
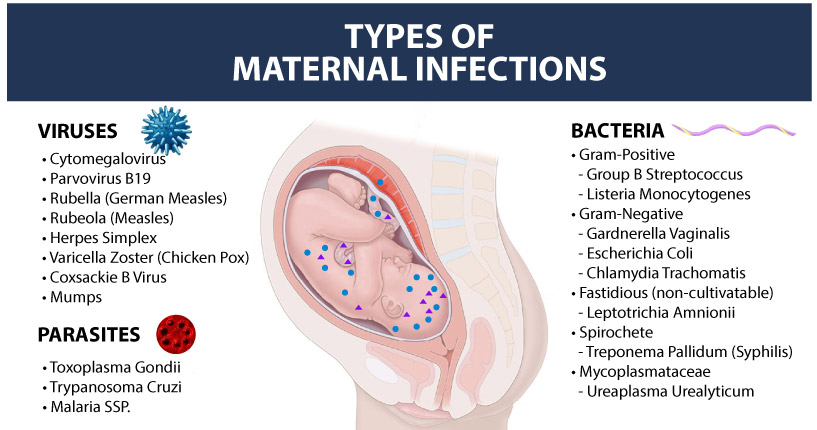
Group B Streptococcus
The most common and preventable infection transmitted by mothers to their babies is Group B strep. Babies that suffer from Group B strep and are not aggressively treated are at high risk for birth injury including brain damage and cerebral palsy.
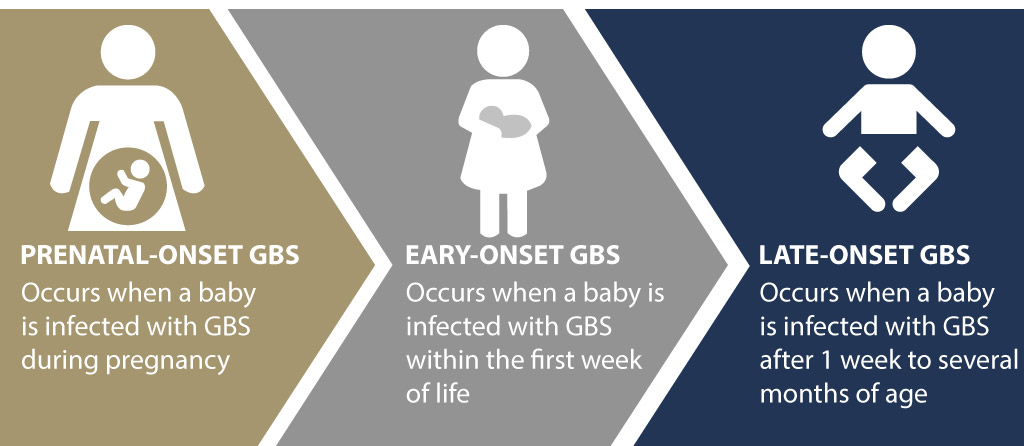
Group B strep (Group B Streptococcus or GBS) is a very common bacterial infection occurring in the genitourinary (genital and urinary) or gastrointestinal (digestive) tract. About one in four pregnant women will have GBS. The majority of these women will have asymptomatic cases.
A pregnant woman infected with GBS can transmit the infection to her baby during vaginal delivery. The primary route of GBS in babies is vertical transmission during passage from the vagina during labor & delivery.
Due to the increased risks GBS poses to expecting mothers and their babies, the CDC recommends screening for all pregnant women for it during the 35th to 37th week of pregnancy.
The top defense against the risk of early onset of GBS infection is timely administration of prophylaxis (preventative) antibiotics to the expecting mother during labor and delivery. As part of routine prenatal testing, medical providers should identify patients that are more likely to benefit from administration of intrapartum (during the birthing process) antibiotics.
Bacterial Vaginosis
Bacterial vaginosis (also known as BV) arises from an imbalance of the typical vaginal bacteria that protects the mother against infections. It is not necessarily a sexually transmitted infection, but it can be spread through sexual contact.
BV affects around 30% of expecting mothers, often without any apparent symptoms. If symptoms do occur, they typically include gray or white vaginal discharge, itching and irritation.
If left untreated, BV can increase a mother’s risk for chorioamnionitis (an infection of the amniotic fluid) and for other urinary tract infections. If the amniotic fluid becomes infected, the baby is at risk for a number of complications including premature birth, low birth weight, and neonatal sepsis.
Expecting mothers with symptoms of bacterial vaginosis should be screened for it using a vaginal pH test or a microscopic examination. Asymptomatic mothers are not routinely screened for BV, but mothers at higher risk for preterm labor should undergo more thorough testing.
Chorioamnionitis
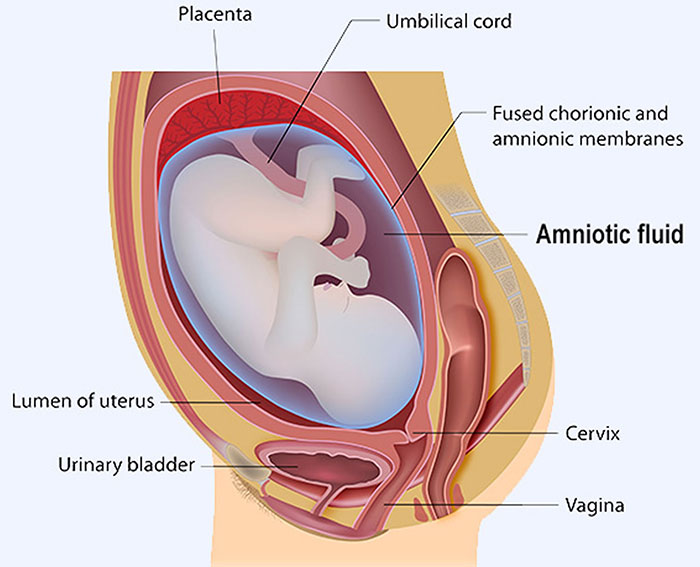
Chorioamnionitis is an acute infection of the mother’s amniotic fluid and membranes that surround her baby in the womb. It typically arises from Group B Strep infections, E. Coli infections, or urinary tract infections that ascend into her uterus either during or shortly before labor.
A mother’s risk for chorioamnionitis increases when her amniotic fluid sac breaks early (known as the premature rupture of membranes or PROM) or when her labor is prolonged or arrested.
A delayed diagnosis or improper management of chorioamnionitis can lead to serious fetal birth complications, such as preterm birth, meningitis, neonatal sepsis, pneumonia, and cerebral palsy.
Medical providers should be prepared to perform an emergency C-section as part of the treatment of chorioamnionitis when necessary. Babies that are born to mothers with a chorioamnionitis infection will often require neonatal resuscitation and immediate antibiotic treatment. During the first hours after birth, doctors and nurses should carefully monitor these babies’ glucose levels and treatment any drops because they are at higher risk for neonatal hypoglycemia.
About Chorioamnionitis Infections
Escherichia Coli (E-Coli)
Escherichia coli (or E. coli) is a group of bacteria that has certain toxic strains to humans (known as Shiga toxin-producing E. coli or Enterohemorrhagic E. coli).
Expecting mothers are highly susceptible to E. Coli infections, particularly urinary tract infections. E. Coli is the most common cause of urinary tract infections during pregnancy, which increases the risk of the bacteria ascending to the uterus and infecting the baby.
While an E. Coli infection is not deadly to the mother, babies who contract it are at higher risk for developing cases of neonatal sepsis or meningitis, which can be life-threatening. They may display mild symptoms of illness beforehand such as fever, vomiting, diarrhea or jaundice.
Maternal E. coli infections can be treated with antibiotic medications and proper hydration and monitoring of symptoms. A timely response is required to mitigate risk, as the infection in rare cases can travel into the bloodstream when left untreated.
Listeriosis
Listeriosis is a foodborne illness caused by the bacteria L. monocytogenes, known plainly as listeria. The CDC estimates that around 1600 people in the U.S. are infected each year, with pregnant women being at the highest risk because of their naturally suppressed immune system.
Doctors can perform a blood test to confirm a case of listeriosis. It typically presents in expecting mothers with flu-like symptoms such as fever, nausea, and muscle aches. If untreated or insufficiently treated, the baby can acquire the infection while in the womb or during or after delivery.
If doctors suspect an expecting mother has been infected with listeriosis, it is critical they act fast because it can cause severe harm if it spreads to her baby. A child who has been infected is at risk for multiple long term complications, including blindness, paralysis, seizures, developmental delays, or impairment to the brain, heart and kidneys.
Toxoplasmosis
Toxoplasmosis is a parasitic infection caused by the parasite known as Toxoplasma gondii. Similar to E. Coli, it is a commonly contracted food-borne illness that is typically acquired through undercooked meat.
The infection poses a heightened risk when acquired during the third trimester. Expecting mothers typically develop flu-like symptoms that aren’t usually severe (though immunocompromised expecting mothers may have harsher symptoms).
When uncaught or insufficiently treated, the parasite can cross the placenta and infect the baby. Reported neonatal symptoms of toxoplasmosis include hydrocephalus (fluid buildup on the baby’s brain) and potential long-term neurodevelopmental disabilities. Some newborns appear unaffected at birth and develop vision impairments or delayed developmental milestones later in childhood after acquiring a congenital toxoplasmosis infection.
Cytomegalovirus
Cytomegalovirus (CMV) is a viral infection that can infect people of all ages, but it can be passed through saliva or from mother to child in the womb. The CDC estimates that around 1% to 7% of expecting mothers will become infected with CMV, and roughly a third of them will pass that infection on to their baby.
Babies with congenital CMV are at a higher risk for hearing loss, seizure disorders, and developmental disabilities. They may show initial signs of rash or jaundice at birth, which are common symptoms.
Once infected with CMV, the virus stays in the mother’s body for life and can reactivate. But compared to most other viral and bacterial infections, the risk of long-term harm to mothers and their newborns from CMV is relatively low. Most people with a CMV infection show zero signs or symptoms, and they often are unaware that they have it. Quick treatment is required for newborns, however, due to their underdeveloped immune system.
Epidural Abscess
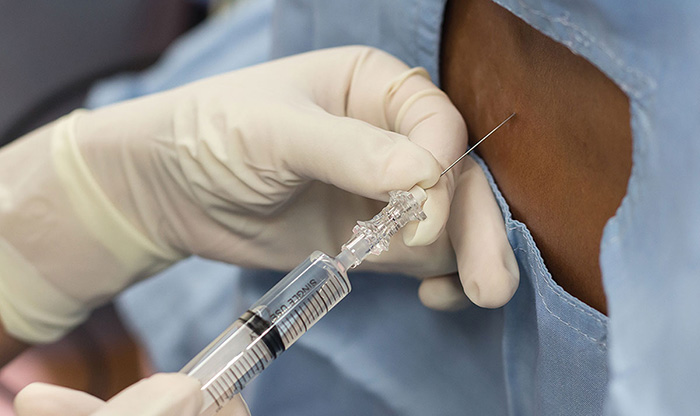
An epidural is a type of regional anesthesia administered to mothers for pain management during labor and delivery.
The epidural typically does not cause any problems for the mother, but complications can occur when she has an underlying bacterial infection. Infections like Group B Strep or Staphylococcus can manifest in the epidural injection site, forming a collection of pus between the spinal bone and the dura matter. This is known as an epidural abscess.
This type of infection is rare but can occur from negligent medical mistakes such as failing to sterilize equipment or properly screen the mother for infections during prenatal testing. When improperly treated, an epidural abscess can lead to permanent spinal cord injury for the mother and even lead to a maternal case of sepsis.
If an epidural abscess is suspected (either from reported back pain or a visible lump around the injection site), doctors should not delay in ordering MRI imaging and blood cultures to confirm it. Surgical drainage followed by antibiotic medication is often required to clear up the infection.
Meningitis Infection
Meningitis is an infection of the thin membranous outer covering of the brain and spinal cord. It is typically caused by another bacterial infection like Group B Strep or E. coli.
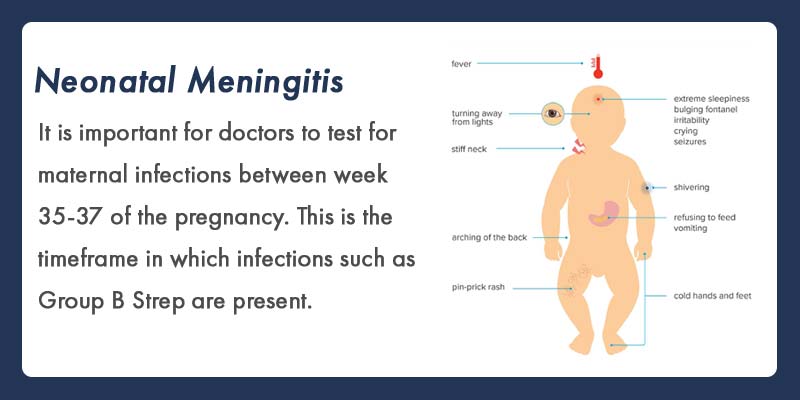
Meningitis is typically not transmitted from mother to child during pregnancy, except in cases of Group B Streptococcus. In theory, any form of harmful bacteria in the mother’s birth canal can increase a newborn’s risk of contracting it.
According to the National Meningitis Association, there are approximately 1,000 cases of meningitis annually, 80% of which affect infants. While meningitis affects people in all age groups, babies with less developed immune systems are particularly susceptible to developing this condition. A premature birth or low birth weight may also contribute to a newborn’s risk of infection.
Medical professionals must provide optimal prenatal care to ensure a healthy delivery, especially during the third trimester. If a doctor fails to recognize and treat the infection promptly, an infected newborn will often require treatment in a neonatal intensive care unit (NICU). Resulting birth injuries from undiagnosed or untreated meningitis can affect a child's quality of life and place a substantial financial burden on the child's family.
Syphilis
Syphilis is a sexually transmitted bacterial infection caused by the bacterium Treponema pallidum. It is often referred to as “the great impersonator” due to its symptoms mimicking those of other infections and diseases.
Having syphilis during pregnancy can be extremely dangerous for the baby. Transplacental transmission can increase the chances of fetal demise or a miscarriage. Maternal health research group March of Dimes reports that up to 2 in 5 babies born to mothers with untreated syphilis die from the infection.
Children who do survive after birth are at a heightened risk for a number of serious birth complications, including jaundice, anemia, bone deformities, and delayed developmental milestones.
All expecting mothers should be thoroughly screened for sexually transmitted infections during prenatal testing appointments in the first trimester. Failing to catch and treat a case of syphilis during this timeframe before it causes complications can constitute medical malpractice in some cases.
Herpes Simplex Virus
Herpes simplex virus (HSV) is a viral infectious disease that causes recurrent painful genital or oral sores. About one in four expecting mothers are positive for HSV type II, though the majority are asymptomatic.
Like other viral infections such as cytomegalovirus, HSV is not curable and will stay dormant within the body throughout one’s life. If the mother has an outbreak during the later stages of pregnancy or during labor and delivery, the infection can pass to the baby. Research suggests the risk of neonatal infection<.a> varies from 30% to 50% for infections that onset in late pregnancy.
Routine screening for HSV during pregnancy is not common, however the mother should inform her healthcare provider if she knows that she is a carrier for the virus. Additionally, if any visible open sores are spotted during a physical examination, doctors may prescribe antiviral medications to treat the outbreak.
Was My Infection Missed or Mismanaged During Pregnancy?

Many common maternal infections such as Group B Strep are routinely screened for during prenatal testing. Medical negligence, such as a misdiagnosis, failure to catch early symptoms an infection, or even operating errors during delivery that directly caused an infection, can worsen a mother’s health and expose their vulnerable baby to dangerous neonatal infections that can result in preventable birth injuries and death.
If a family believes medical negligence contributed to a child’s infection-related injury, legal support may be an option. A specialized birth injury attorney can review the medical records and circumstances to assess whether a claim exists.
Parents whose children suffer from the long-term effects of birth complications, as well as parents who have suffered the loss of their baby, deserve to know whether it could have been prevented. Our dedicated birth injury lawyers want to help you find those answers and obtain the funds necessary to improve the quality of life for your child.
If your child has been diagnosed with a birth injury and you suspect this may have been caused in part by medical mistakes, Miller Weisbrod Olesky will thoroughly investigate the facts and hold the responsible medical providers accountable by pursuing medical malpractice claims against them.
Sometimes families are hesitant to reach out to a medical malpractice attorney or law firm. They may feel overwhelmed by their circumstances or are worried that a law firm will not be able to help them. But the only way to find out if you have a case is to talk to an attorney who understands how birth injuries can lead to developmental delays and other complications that require long-lasting medical support.
Birth Injury Malpractice: Statute of Limitations

A statute of limitations is a law that imposes a deadline for filing birth injury lawsuits. If you fail to file a claim before the statute of limitations "runs out", you may lose your right to pursue legal action and seek compensation. In some cases where an injury may not be immediately apparent, the statute of limitations may be extended.
The discovery rule prevents the statute of limitations from running until the injury is discovered or reasonably should have been discovered. It is also important to remember that the statute of limitations varies by state and the type of claim you're filing. A birth injury attorney can help you avoid missing all crucial deadlines related to your case.
How Can Our Birth Injury Attorneys Help?

It takes a detailed expert review of the facts and circumstances of your pregnancy and your child's birth before determining whether an uncaught or insufficiently treated infection resulted in a preventable birth injury or infant wrongful death.
Our Process
At Miller Weisbrod Olesky, a team of committed attorneys, nurses and paraprofessionals uses our detailed medical negligence case review process to assess your potential birth injury case. We start by learning more about you and your child and the status of meeting/missing developmental milestones. Then we gather medical records to determine what happened before, during, and after your delivery.
We call in skilled medical experts who review your records and let us know if they think medical errors could have caused your child's injuries. If we believe medical negligence was a legitimate contributing factor to your uncaught maternal infection and any resulting complications, we will meet with you to discuss how you can receive compensation from the medical professionals who made the errors.
At no point in our legal intake process will we ask you to pay anything. The medical review of your case and the consultation are free. We only receive payment once you do. The sooner you reach out to us, the sooner we can begin investigating your case and gathering the evidence needed to support your claim.
We work on a contingency fee basis, meaning you won't pay any legal fees unless we win your case. Contact us today to schedule your free legal consultation by calling our toll-free line at (888) 987-0005 or by filling out our online request form.
Contact Our National Birth Injury Lawyers
National Birth Injury Law
Our National Birth Injury Attorneys, nurses, and support staff understand that parents of children with birth injuries feel overwhelmed. So, every client has the attention and support of a team of trained, compassionate professionals. But we don’t just offer compassion.
We offer a process to help you discover whether your child’s birth injury, HIE, cerebral palsy or brain injury at birth was caused by medical malpractice.
Call our offices today at (888) 987-0005 for experienced assistance in a free consultation.
Quick Links
Testimonials
- Lyric C. I feel like our voice was heard in a sense of what can possibly go wrong in a delivery and finding us answers. I feel with our settlement, we are now in a comfortable position to provide for our son.
- Lyssa L. They are not just people that say “hey let's get you money and let's go” The law firm was very thorough with us. It was awesome. I don't want to cry, because I think about and it's amazing that they were able to help me and that we were able to help my son and get the story out there.
- Jay C. Throughout the process, one thing was clear to us, the ultimate interest of our child was the utmost concern of Max and his team and as parents navigating a situation like that, that was refreshing to know we had them firmly on our side. I highly recommend them.
Popular Cities
- ★ Dallas Birth Injury
- ★ Houston Birth Injury
- ★ Atlanta Birth Injury
- ★ Chicago Birth Injury
- ★ Philadelphia Birth Injury
Locations
★ Dallas
11551 Forest Central Drive, Ste. 300
Dallas, TX 75243
★ Houston
12929 Gulf Freeway, Ste. 111
Houston, TX 77034