Hypoxia & Anoxia
What is Hypoxia and Anoxia?
Oxygen deprivation is the predominant cause of brain damage in newborns. These are the most devastating types of birth injuries because they often come with lifelong, irreversible conditions and complications.
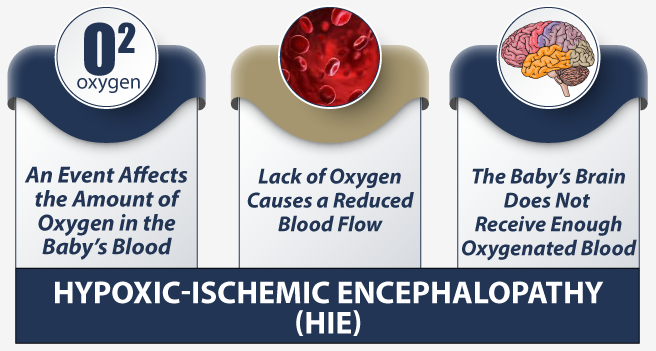
Many babies who suffer from hypoxia and anoxia in the perinatal phase (shortly before and after birth) develop brain injuries. The most common hypoxic brain injury is hypoxic ischemic encephalopathy (HIE), which stems from reduced blood flow to the brain.
HIE is a permanent condition that can cause developmental delays, seizures and epilepsy, vision impairments, speech impairments, and other disabilities. HIE is the leading cause of cerebral palsy in early childhood.
Oxygen deprivation poses a critical threat to the baby’s overall wellbeing. Doctors, nurses, and other present medical staff must remain vigilant during labor and delivery while observing the child’s vital signs. They should always keep careful watch of electronic fetal heart rate monitoring strips and any labor complications that may arise.
Failing to adequately identify and manage hypoxia and anoxia at birth can cause devastating injuries and may constitute medical malpractice.
Birth Injury Malpractice Attorneys
Our top rated birth injury attorneys specialize in identifying how oxygen deprivation during delivery can lead to severe brain injuries. If your baby suffered from hypoxia and anoxia at birth, don’t hesitate to contact our firm. We can answer difficult legal and medical questions and investigate the facts on your behalf.
Free Legal Consultation
Birth Injury Lawyers
(888) 987-0005Our Birth Injury Lawyers are available to meet you in your home or the hospital.
Our vast network of medical experts and in-house nursing staff and nurse-attorneys gives us the edge over our competition. When we take your case, we assign you with not just an attorney but an entire medical team. This team includes attorneys, experienced nursing advocates, and seasoned medical experts.
Your team is available to assist with any day-to-day treatment you or your child may need. This includes assistance with obtaining medical records, scheduling doctors’ appointments, providing transportation, and any other problems that may arise.
We offer all of this on a contingency fee basis. This means you will not pay any fees until after we win your case and secure a settlement. Our unmatched track record of birth injury results sets us apart from other birth injury law firms.

Recent Birth Injury Settlement:
Birth Injury settlement against a hospital in which nurses and physicians failed to properly monitor the mother's blood pressure during delivery causing an HIE event resulting in neonatal seizures and cerebral palsy at birth. Our team of top-rated birth injury lawyers recovered $13,750,000 for the family to help with future medical expenses and developmental therapy.
What is Hypoxia?
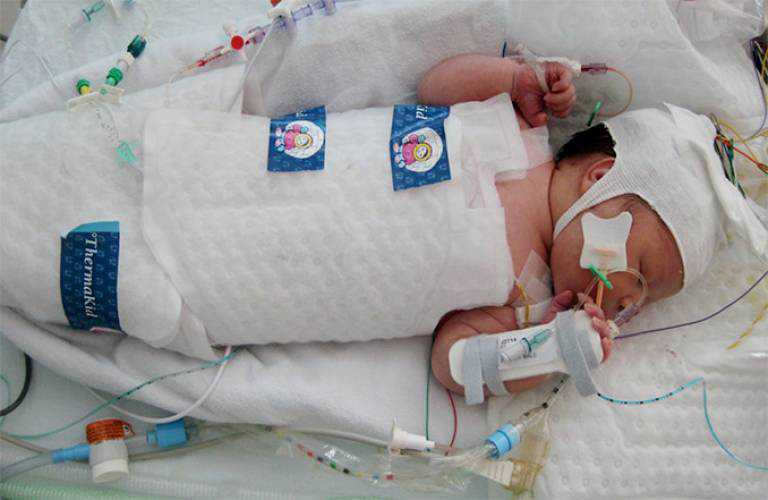
Hypoxia is a condition where the body’s tissues do not have enough oxygen.
Humans initially inhale oxygen through their lungs. The oxygen passes through the alveoli (tiny air sacs within the lungs) and then dissolves into the bloodstream. The oxygenated blood travels to the heart, which then pumps it back out to the rest of the body’s tissues.
The cells inside the body’s tissues depend on oxygen to produce energy and function properly. Without it, they may begin to shut down. This is how hypoxia can lead to brain damage.
Hypoxia can develop into anoxia, which is a complete lack of oxygen in the tissues. A baby with anoxia is likely to suffer from organ damage.
How does Hypoxia and Anoxia Occur During Labor and Delivery?
Many factors or even a combination of factors can contribute to a child’s oxygen deprivation at birth. The primary cause of hypoxia and anoxia in newborns is birth asphyxia.
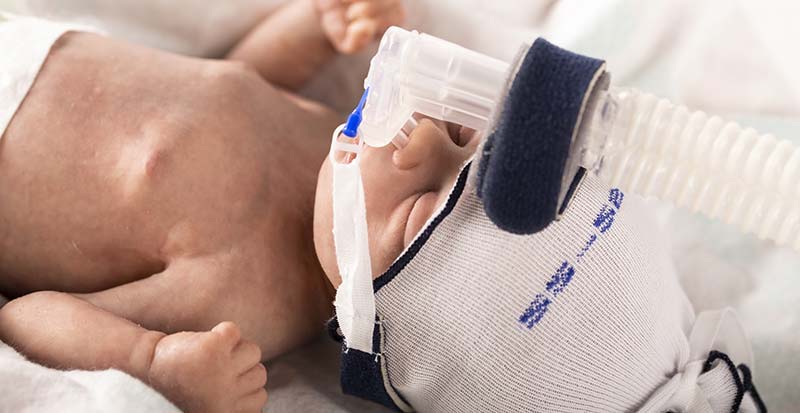
Birth asphyxia is the term for when any type of blockage obstructs oxygenated blood from reaching the baby’s brain. Many different labor and delivery complications can cause this, including:
Hypoxia and anoxia may also occur due to ischemia (obstruction) or ruptured blood vessels. This can happen due to abnormal functioning of the heart valve or abnormal pulmonary functioning.
What Are Risk Factors for Hypoxia?
A risk factor for hypoxia is any complication that could indirectly pose a threat to the baby’s oxygen supply. These complications increase the risk for blockages that cause birth asphyxia and ultimately lead to hypoxic brain injuries.
Hypoxia Risk Factors During Pregnancy

Pregnancy complications and other risk factors that could result in fetal oxygen deficiency include:
Hypoxia Risk Factors During Labor
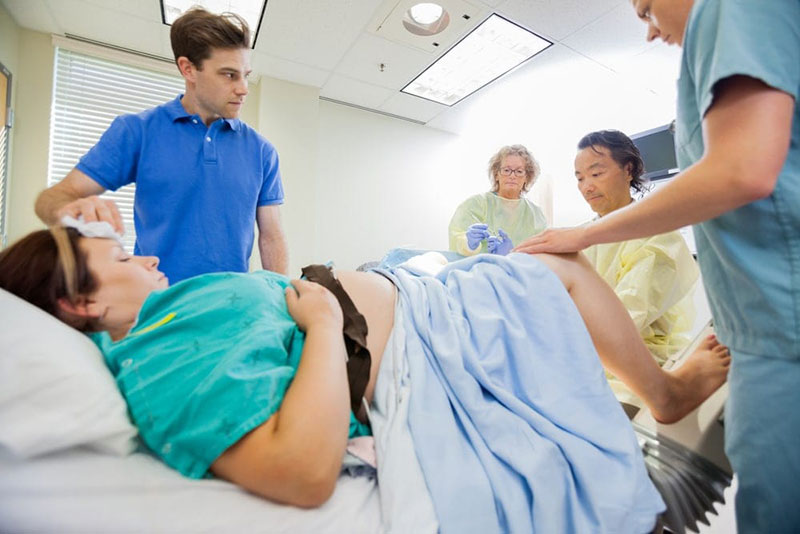
Labor and delivery complications can also threaten a baby’s oxygen supply. The most common risk factors for hypoxia and birth asphyxia during labor include:
Mismanaging birth complications after delivery can also increase a baby’s risk for hypoxia. Errors during resuscitation or other forms of neonatal breathing mismanagement such as overventilation can lead to brain damage at birth.
What Are Symptoms of Hypoxia and Anoxia?
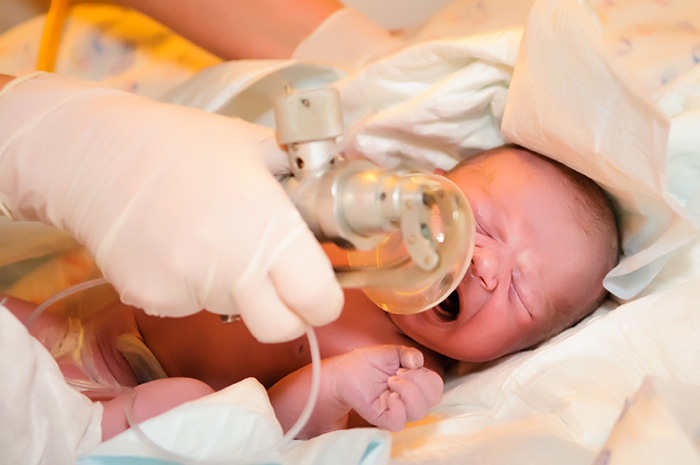
A baby suffering from hypoxia will show signs of oxygen deprivation even before they are born. Some of the common signs of symptoms of hypoxia both during pregnancy and after birth include:
Fetal Distress

One of the first indicators of hypoxia and anoxia during labor is a change in the heartrate. This is notable from an irregular or erratic heart rate.
Fetal heart rate monitoring is vital at the time of labor as well as after labor to make sure that the baby is getting adequate oxygen. Doctors should raise concern when the strips show a low heart rate (bradycardia), late decelerations, or a decrease in variability.
Medial intervention is necessary when doctors observe prolonged non-reassuring fetal heart rates. This can start with small adjustments and ultimately include an emergency C-section if conditions do not improve.
Low APGAR Scores

The APGAR test is a routine, standardized assessment of a newborn’s physical qualities immediately upon delivery. Medical professionals award 0-2 “points” while evaluating the baby’s Appearance, Pulse, Grimace, Activity, and Respiration.
A baby who has suffered from hypoxia will likely score low for all categories, especially for Respiration and Pulse. But it’s important to note that medical bias and subjectivity can interfere with the APGAR score’s reliability.
Respiratory Distress Syndrome
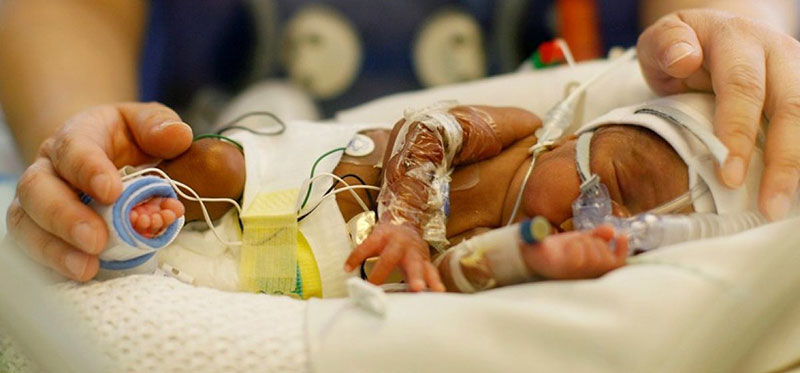
Babies with underdeveloped lungs can go into respiratory distress upon birth. Symptoms can include rapid and shallow breathing, flared nostrils, and a blueish hue around the baby’s lips, fingers, and toes.
Babies suffering from oxygen deprivation will likely meet the criteria for respiratory distress syndrome at birth. This is a sign that they will require assisted ventilation or even possibly neonatal resuscitation.
Fetal Acidemia
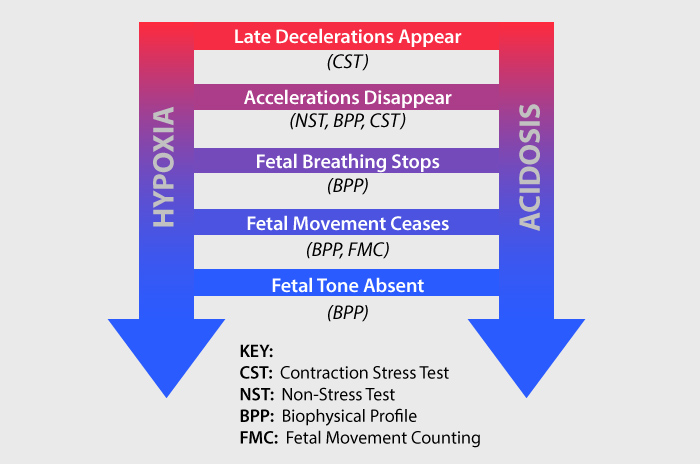
Babies who suffer from oxygen deprivation may have an excess amount of carbon dioxide in their blood as a result. Because carbon dioxide is acidic, too high of a concentration can throw off the baby’s blood pH balance.
Dangerously low pH levels below 7 can classify a baby as “acidotic,” resulting in multiple potential complications. Babies who suffer from fetal acidosis are at a higher risk for brain damage at birth.
Meconium Aspiration Syndrome
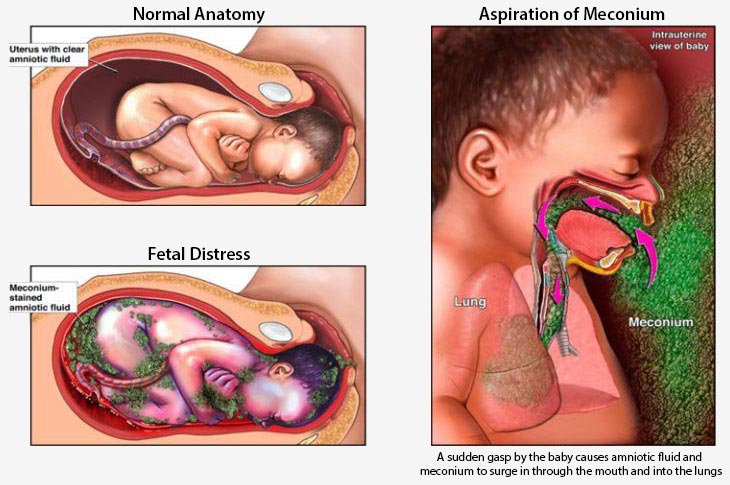
Meconium is the baby’s first stool. It typically lines the baby’s intestines but can sometimes mix in with the amniotic fluid in the womb.
If a baby is already in fetal distress, a sudden gasp for air could cause them to inhale meconium-stained fluid. This can be dangerous if the meconium enters the baby’s lungs and blocks their airways.
Meconium aspiration syndrome increases the baby’s risk for asphyxia, hypoxia, and respiratory distress.
Neonatal Seizures
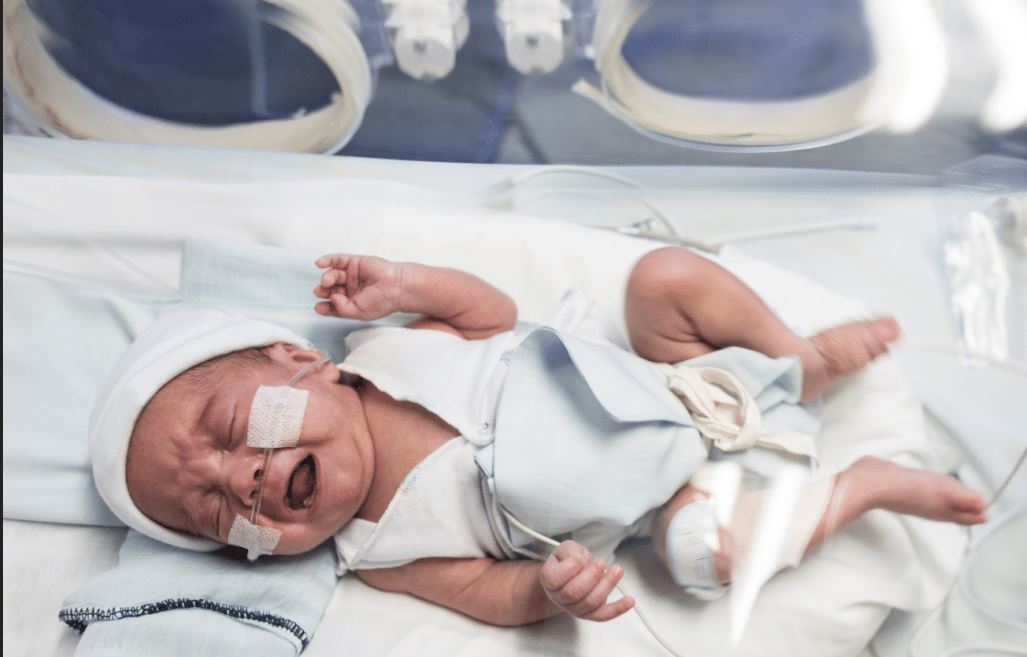
Neonatal seizures may occur when the brain fails to receive oxygen for a prolonged period. In this condition, the brain will go into an emergency mode until it begins to malfunction. This is when seizures may develop.
Additional symptoms of hypoxia and anoxia at birth may include:
- Fatigue or lethargy (low movement)
- Weak or poor muscle tone
- Yellowish color (Jaundice)
- Absence of crying or weak crying
- Absence of urination
- Poor reflexes
- Low blood pressure
Signs of Brain Damage During Childhood

Some signs of hypoxia and resulting injuries may not appear until the child is older. Parents should be mindful of the following signs, among others, in these cases:
- Cerebral palsy
- Developmental delays
- Movement disorders
- Balance problems
- Speech difficulties
- Visual impairment
- Hearing impairment
- Epilepsy
How to Detect Hypoxic Brain Damage?
Medical professionals can use multiple tools and strategies to identify hypoxia and any resulting brain damage. The most common diagnostic methods include:
Fetal Heart Monitoring
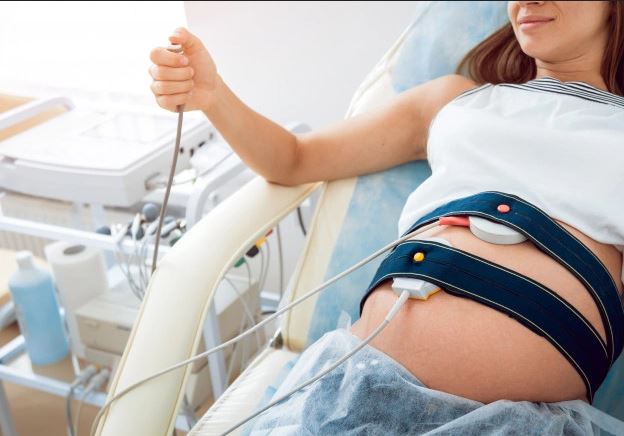
Fetal heart rate monitoring is an important tool for medical providers to gather critical insights into the baby’s oxygen supply.
Careful monitoring will usually help them detect abnormal heart rates to implement a timely treatment plan. If the infant is at the risk of hypoxia and anoxia during labor, they may go ahead with an emergency C-section.
Umbilical Cord Blood Gas Testing
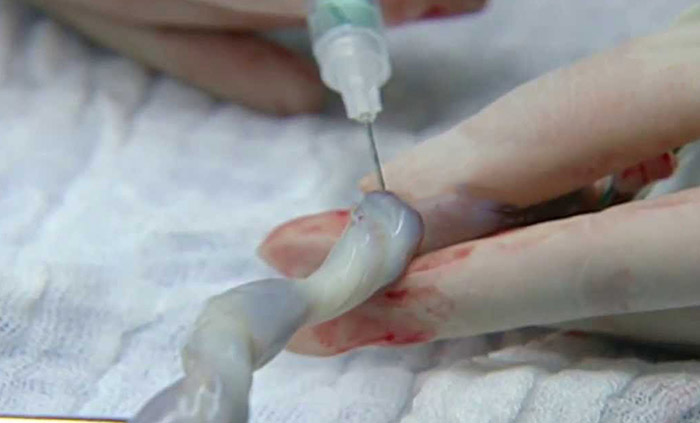
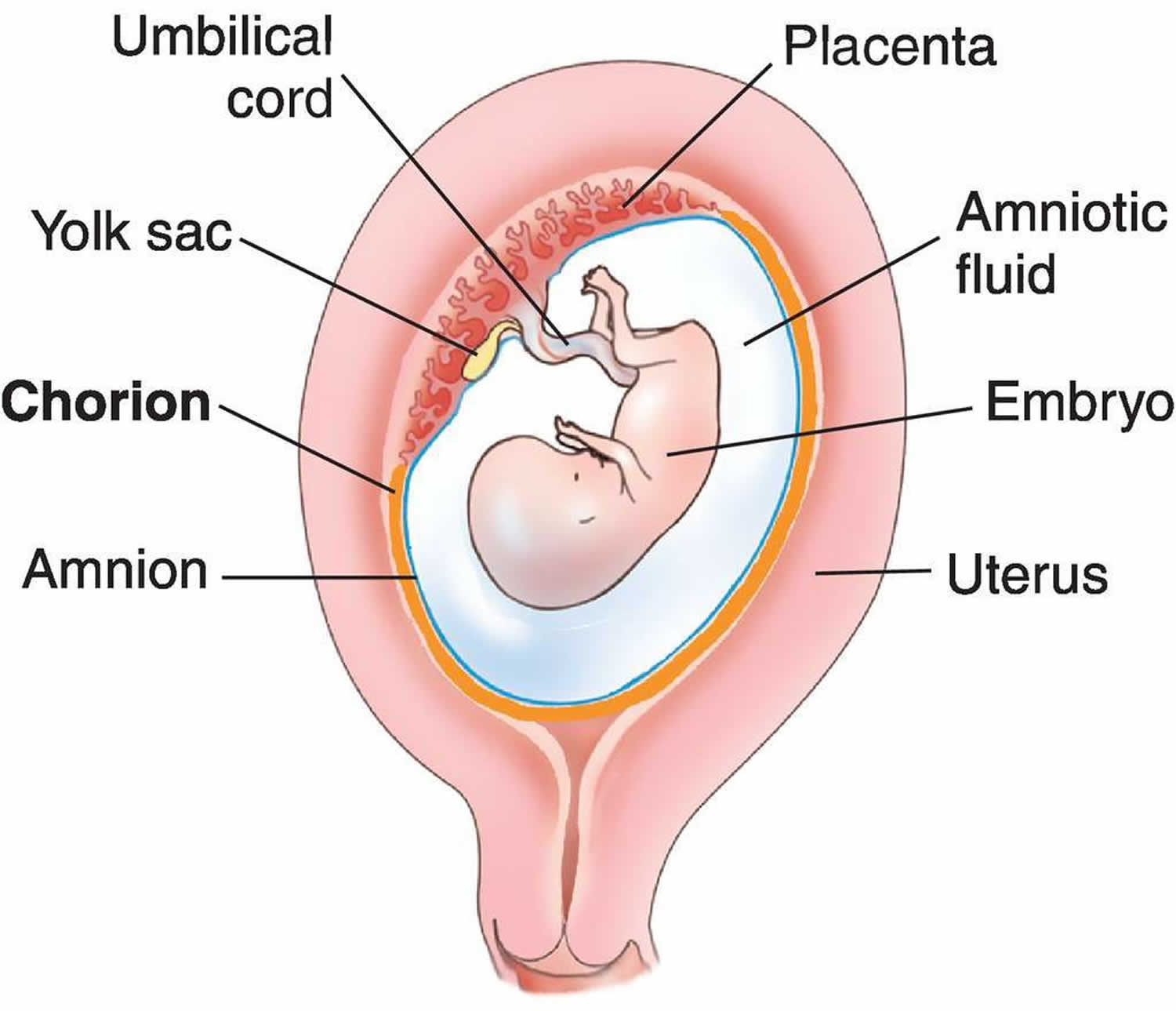
During pregnancy, the baby receives all oxygen from blood that flows through the umbilical cord vein. The umbilical cord arteries remove carbon dioxide from the baby’s system and return it back to the placenta.
Analyzing umbilical cord blood samples after birth can determine if the baby suffered from birth injuries like hypoxia or birth asphyxia. If the sample reveals low levels of oxygen, medical professionals should move forward with further testing for brain injuries.
About Umbilical Cord Blood Gas
Neonatal Neuroimaging
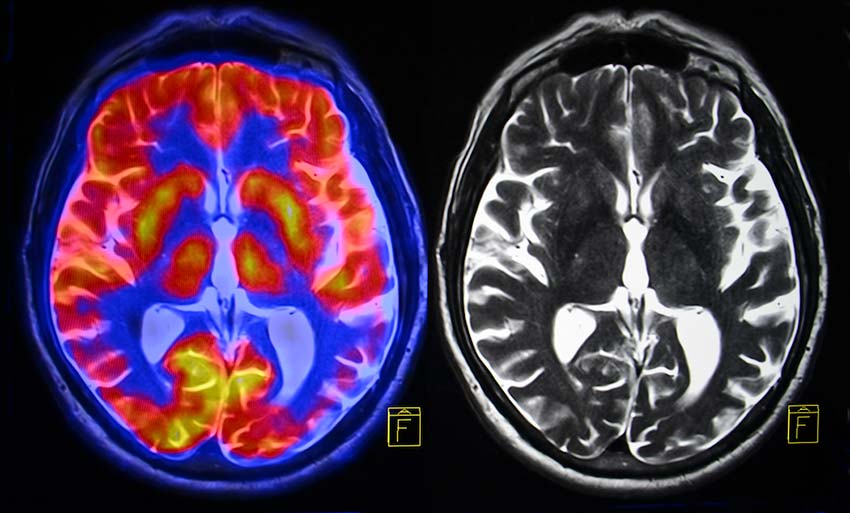
Medical professionals can confirm a brain injury related to hypoxia and anoxia by performing neuroimaging tests after birth. Tests may include an EEG (electroencephalogram), MRI (magnetic resonance imaging) and/or a Head CT (computerized tomography) scan.
Neuroimaging can reveal different hypoxic brain injury patterns that match for cases of hypoxic ischemic encephalopathy or for periventricular leukomalacia. It can also alert doctors to which parts of the brains received damage, which can help them accurately predict symptoms.
What Is The Prognosis for Hypoxia and Anoxia?
Children with hypoxia during pregnancy or at birth may suffer permanent or severe brain damage including HIE and cerebral palsy. The prognosis can vary according to the severity of brain damage, co-morbidities (other health conditions), and the child’s general health. The extent of damage usually depends on:
- The degree/level of oxygen deprivation
- How long the oxygen deprivation lasted
- How quickly doctors provided the right treatment
Newborns that experience HIE (hypoxic ischemic encephalopathy) are more likely to suffer permanent long-term conditions, such as cerebral palsy. Birth asphyxia may also affect other organs, apart from the brain, such as the heart, kidneys, lungs, and bowels. In extreme cases, total organ failure or the death of the baby may occur.
Children who experience permanent organ damage usually need extensive care and birth injury treatment. This can include lifelong therapy and medications, constant supervision, and special education.
How to Treat Hypoxia After Birth?
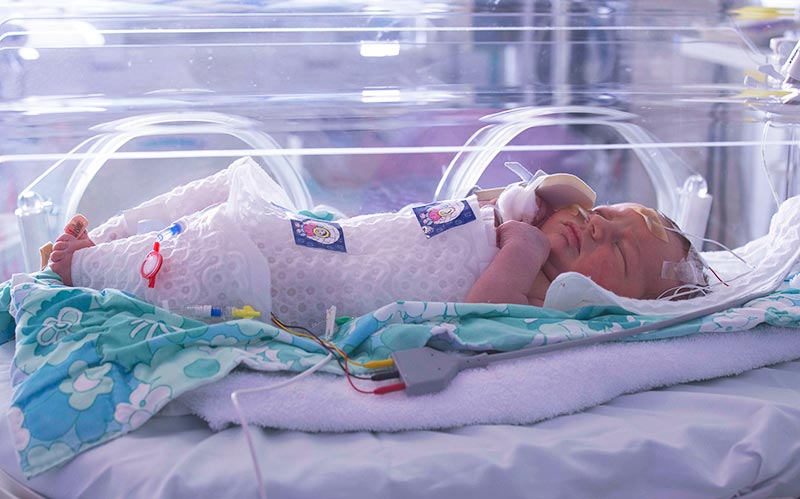
If an infant has mild asphyxia at the time of birth, the medical team should perform initial stabilization maneuvers. These can include head repositioning, tactile stimulation, and nose and mouth suctioning.
Doctors must intervene further when the baby suffered a more severe hypoxic or anoxic brain injury. The proper neonatal resuscitation methods include:
- Supplemental oxygen
- CPAP – continuous positive airway pressure
- NIPPV – noninvasive positive pressure ventilation
- Intubation Mechanical ventilation or bag & mask ventilation
Medical providers should order a full cardiac evaluation to rule out any congenital cardiopulmonary defects. At the same time, more advanced treatments or treatment combinations that doctors may consider implementing includes:
High Frequency Oscillatory Ventilation (HFOV)
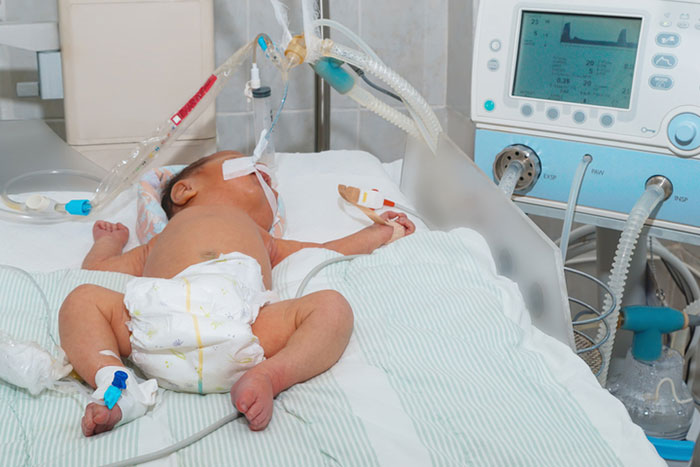
This ventilatory technique provides breathing support to the infant from a machine that uses pressure oscillations to deliver low-volume but rapid puffs of air into the baby’s lungs. The mechanism is gentler than a standard breathing machine to ensure that the delicate lungs of the newborn do not suffer any damage from high airway pressure.
Inhaled Nitric Oxide
If the newborn has pulmonary hypertension (high blood pressure in the lungs), doctors may use inhaled nitric oxide. The infant will receive the gas into their airway through a heart-lung pump or a breathing tube for life support. This will enable dilation (opening) of the blood vessels in their lungs so they can take in more oxygen.
Therapeutic Hypothermia
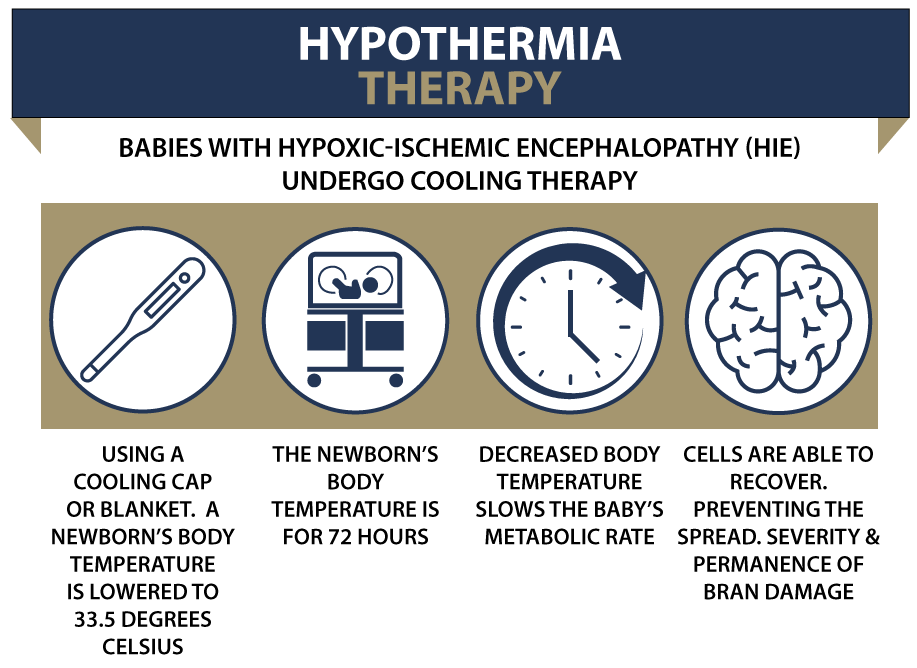
Hypothermia therapy can help protect the infants who have suffered HIE injury from further damage. Medical providers should ideally start this treatment within six hours after birth to minimize brain damage.
The therapy involves cooling the infant’s internal body temperature to about 91°F for a period of 72 hours. Doctors should only apply brain cooling when the infant’s gestational age is 35 weeks or more. Administering this treatment to premature babies can risk further injury.
Did Medical Errors Cause My Child’s Hypoxia at Birth?

Hypoxia and anoxia can cause brain injuries like HIE and other neurological outcomes that will forever alter a child’s life. Birth injury negligence, like delaying a C-section amid fetal distress or delaying therapeutic hypothermia after birth, increases the baby’s risk.
If a family believes medical negligence worsened a child’s brain damage at birth, legal support may be an option. A specialized birth injury attorney can review the medical records and circumstances to assess whether a claim exists.
Families who have experienced the effects of hypoxic brain injuries from negligent medical care deserve to know whether they were avoidable. Our top rated birth injury lawyers will help you find those answers and obtain the necessary funds to secure treatment.
Our National Birth Injury team will thoroughly investigate the facts, holding responsible parties accountable by pursuing medical malpractice claims.
What is the Statute of Limitations in a Birth Injury Lawsuit?

A statute of limitations (SOL) is a law that sets a time limit on how long an injured person has to file a lawsuit after an accident. It is essential to understand that statutes of limitations vary based on the case and the state where you file. For instance, the deadline for birth injury claims is typically different from other claims, such as injury to private property.
Generally, the clock starts ticking on the date the injury occurred. However, there are exceptions to this rule. In some cases, the statute of limitations starts when a person discovers or reasonably should have discovered an injury. When dealing with government agencies, SOLs can become even more complex.
For example, if the party that injured you was:
- A federal employee
- Employed by a military hospital, Veterans Administration facility, or a federally funded medical entity
You may need to file a birth injury claim under the Federal Tort Claims Act (FTCA). In FTCA cases, claimants must go through certain administrative procedures before filing a lawsuit. In some states, you may have less time to give notice if:
- The negligent party was a local or state government hospital.
- The doctors and medical providers are employees of a governmental entity.
If you file your case outside of the statute of limitations, the court will typically dismiss it. This means you will not be eligible to recover compensation for you or your child’s injuries.
Determining when a statute of limitations begins on your case can be tricky. If you are considering pursuing compensation, contact a birth injury attorney as soon as possible.
How Can Our Birth Injury Attorneys Help?

Doctors can sometimes prevent fetal hypoxia by taking quick action in response to non-reassuring fetal heart rates. However, it takes an expert review of the facts of your birth to determine whether medical professionals made preventable errors.
Our Process
Our team of committed attorneys, nurses and paraprofessionals works to answer these questions and seek compensation. We use our detailed medical negligence case review process to assess your potential birth injury case.
We start by learning more about your pregnancy by gathering records to determine what happened during and after your delivery. This includes evaluating the fetal heart rate strips during labor and umbilical cord arterial blood gas testing procedures after birth.
We will call in skilled medical experts who review your records and provide insight into where medical professionals went wrong. If we feel medical negligence caused or worsened your baby’s hypoxia, we meet with you to discuss further.
At no point in our legal intake process will we ask you to pay anything. The medical review of your case and the consultation are free. We only receive payment once you do. The sooner you reach out, the sooner we can investigate your case and gather the evidence to support your claim.
We work on a contingency fee basis, meaning you will not pay any legal fees until we win your case. We do not purse any medical malpractice cases unless we fully believe we can win.
Contact us today to schedule your free consultation by calling our toll-free line at (888) 987-0005. You can also reach us by filling out our online request form.
National Birth Injury Law
Our National Birth Injury Attorneys, nurses, and support staff understand that parents of children with birth injuries feel overwhelmed. So, every client has the attention and support of a team of trained, compassionate professionals. But we don’t just offer compassion.
We offer a process to help you discover whether your child’s birth injury, HIE, cerebral palsy or brain injury at birth was caused by medical malpractice.
Call our offices today at (888) 987-0005 for experienced assistance in a free consultation.
Quick Links
Testimonials
- Lyric C. I feel like our voice was heard in a sense of what can possibly go wrong in a delivery and finding us answers. I feel with our settlement, we are now in a comfortable position to provide for our son.
- Lyssa L. They are not just people that say “hey let's get you money and let's go” The law firm was very thorough with us. It was awesome. I don't want to cry, because I think about and it's amazing that they were able to help me and that we were able to help my son and get the story out there.
- Jay C. Throughout the process, one thing was clear to us, the ultimate interest of our child was the utmost concern of Max and his team and as parents navigating a situation like that, that was refreshing to know we had them firmly on our side. I highly recommend them.
Popular Cities
- ★ Dallas Birth Injury
- ★ Houston Birth Injury
- ★ Atlanta Birth Injury
- ★ Chicago Birth Injury
- ★ Philadelphia Birth Injury
Locations
★ Dallas
11551 Forest Central Drive, Ste. 300
Dallas, TX 75243
★ Houston
12929 Gulf Freeway, Ste. 111
Houston, TX 77034