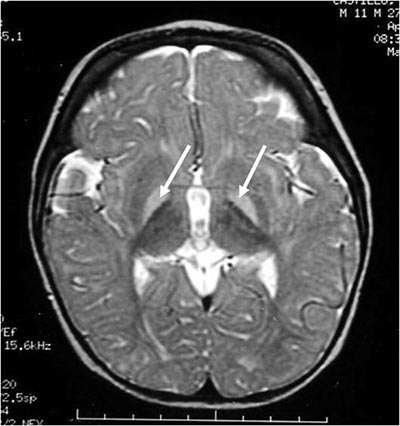
Jaundice and Kernicterus
Newborn Jaundice and Kernicterus
A Common Condition that Can Lead to Infant Brain Damage
A baby’s yellowish skin pigment at birth can be frightening for many parents. They may worry that their child is in pain or battling a serious health condition. But this yellow discoloration is very common and highly treatable when competent medical professionals react to it in time.
Neonatal jaundice often occurs when the baby’s liver struggles to break down waste products in the bloodstream. The condition typically resolves itself as their liver matures. But when an underlying birth complication is causing the baby’s liver dysfunction, this seemingly harmless condition can quickly turn serious.
Untreated jaundice can leave high traces of waste called bilirubin in the baby’s bloodstream. If this waste travels to the brain, it can cause irreversible brain damage at birth known as kernicterus. Kernicterus can cause permanent disabilities, including hearing loss, developmental delays, and multiple forms of cerebral palsy.
Doctors, nurses, and other attending medical professionals should be able to discern between mild and severe cases of jaundice. They should understand how risk factors like prematurity, neonatal infections, and blood type incompatibility increase a baby’s risk for kernicterus.
If your jaundiced baby sustained preventable brain injuries because healthcare providers failed to intervene, it can qualify as medical malpractice. Our Jaundice Birth Injury Lawyers can help you determine whether better treatment could have prevented your baby’s kernicterus diagnosis.
Birth Injury Malpractice Attorneys
Our top rated birth injury attorneys specialize in helping families seek justice and compensation for preventable injuries during birth. If your baby suffered brain damage from untreated jaundice that progressed into kernicterus, do not hesitate to reach out. We can help you assess the strength of your claim and whether your family is eligible to recover financial damages.
Free Legal Consultation
Birth Injury Lawyers
(888) 987-0005Our Birth Injury Lawyers are available to meet you in your home or the hospital.
Our firm’s vast network of medical experts, in-house nursing staff, and nurse-attorneys gives us the edge over our competition. When we take your case, we assign you with not just an attorney but an entire medical team. This team includes attorneys, experienced nursing advocates, and seasoned medical experts.
While your case is ongoing, your team will help you with the day-to-day treatment you or your child will need. This includes assistance with obtaining medical records, scheduling doctors’ appointments, providing transportation, and any other problems that may arise.
We offer all of this on a contingency fee basis. This means you will not pay any fees until after we win your case and secure a settlement. When we win, we will only charge a pre-agreed percentage in fees from your settlement or jury award. We offer free legal consultations and will happily take your call to answer any pressing legal questions free of charge.
Our national birth injury team has a track record of birth injury results sets us apart from other firms.

Recent Birth Injury Settlement:
Birth Injury settlement against a hospital in which nurses and physicians failed to properly monitor the mother's blood pressure during delivery causing an HIE event resulting in neonatal seizures and cerebral palsy at birth. Our team of top-rated birth injury lawyers recovered $13,750,000 for the family to help with future medical expenses and developmental therapy.
What are Jaundice and Kernicterus?
Newborn jaundice is a condition where the baby’s skin and eyes develop a yellowish tint shortly after birth. The substance responsible for the yellow discoloration is bilirubin.
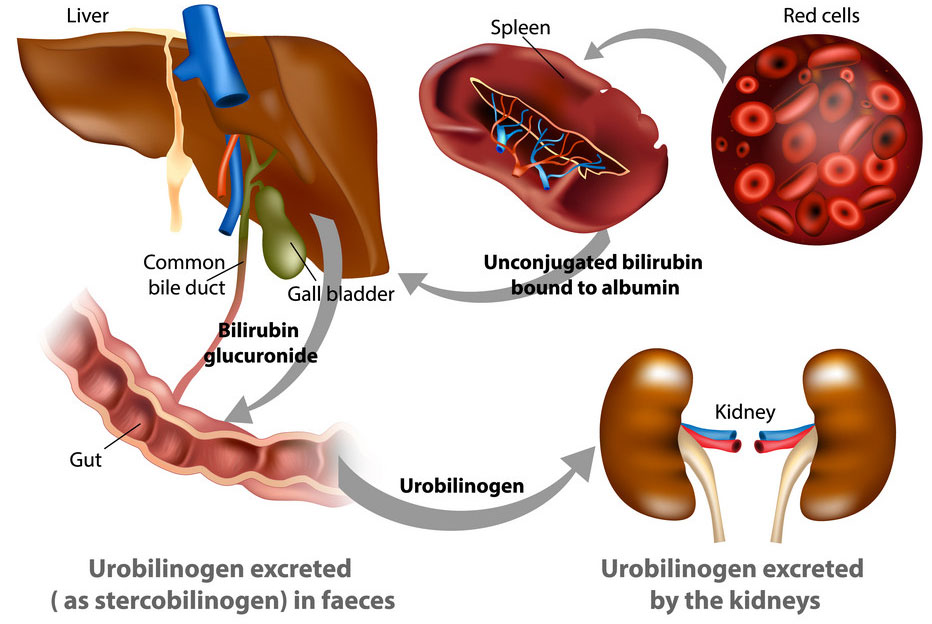
What is Bilirubin?
Bilirubin is a yellow-orange substance found in the bloodstream. It is a waste product that the body naturally creates after breaking down old red blood cells. When the body processes it properly, bilirubin aids in the digestion process by breaking down fats and eliminating other waste.
Bilirubin appears in the bloodstream as a byproduct of the body breaking down and recycling red blood cells. It travels through the blood to the liver for processing.
During pregnancy, the mother’s liver processes all the baby’s bilirubin for them. But after birth, the baby must rely entirely on their own liver to process it. Many newborns have trouble with this because their liver has not yet fully matured.
If the baby’s liver is too underdeveloped to process bilirubin, the substance will begin to accumulate in the bloodstream. High concentrations of bilirubin in the blood (called “hyperbilirubinemia”) will give the baby’s skin the yellow hue indicative of jaundice.
Hyperbilirubinemia can be dangerous if it reaches the brain. When high bilirubin levels cross the blood-brain barrier, it can cause a form of brain damage called kernicterus. Kernicterus brain injuries cause permanent neurological damage, often resulting in hearing loss, cognitive impairments, and movement disorders like cerebral palsy.
How Common is Jaundice in Newborns?
Neonatal jaundice is a relatively common condition. Around 60% of full-term newborns will develop hyperbilirubinemia causing yellow skin discoloration within the first week of birth.
Babies born prematurely are even more likely to experience jaundice; up to 80% of premature newborns will develop the condition. Premature babies have a higher risk for jaundice because their organs have had even less time to mature and develop.
Kernicterus, on the other hand, is a far rarer condition. One analysis estimates that around 7 in 100,000 newborns will develop bilirubin levels high enough to cause brain injuries.
Despite the low incidence, medical professionals should never rule out a jaundiced baby’s risk for kernicterus.
Bilirubin: Conjugated vs. Unconjugated
While discussing a baby’s jaundice, you may hear doctors use terms like “unconjugated bilirubin” and “conjugated bilirubin.” These medical terms may sound complex, but they have simple meanings:
Unconjugated Bilirubin
Bilirubin that the liver has not yet processed. Unconjugated bilirubin is highly toxic for newborns because it is lipid-soluble, meaning it can travel through cellular membranes. This quality is what allows unconjugated bilirubin to cross the blood-brain barrier and cause kernicterus.
Conjugated Bilirubin
Bilirubin that the liver has processed. Conjugated bilirubin (also sometimes called “direct” bilirubin) is water-soluble and not toxic to the body’s tissues. The body uses conjugated bilirubin to make bile, which helps break down fats in the foods we eat.
The concentration of each type of bilirubin can indicate the extent of the baby’s jaundice and their risk for kernicterus. Elevated bilirubin levels should concern any medical professional, particularly when caring for a newborn.
What Causes Jaundice in Babies?
The most common cause for high bilirubin levels is the baby’s immature liver being unable to process it quickly enough. Doctors typically refer to these cases as “physiological jaundice,” which is the most harmless type. Physiological jaundice almost always self-corrects as the baby’s internal organs strengthen with age.
But multiple other birth complications and conditions can cause elevated bilirubin levels in the blood. These include:
Blood Type Incompatibility

Everyone’s blood has a type: A, B, AB, or O. Additionally, some people have a protein called the Rhesus factor (Rh factor) on the surface of their red blood cells. The presence or absence of this Rh protein will determine whether your blood type is positive (+) or negative (-).
Rh and ABO incompatibility occurs during pregnancy when the mother’s blood type or Rh factor differs from her baby’s blood. When small traces of incompatible fetal blood enter the mother’s circulation, her immune system will register it as a threat.
The mother’s body will create antibodies as a response to the foreign fetal blood. These antibodies enter the baby’s circulation through placental blood flow exchange and begin rapidly attacking their red blood cells.
As the antibodies break down the baby’s red blood cells, it will release excess amounts of bilirubin into their bloodstream. Heightened bilirubin levels can lead to jaundice at birth and an increased risk for kernicterus.
Anemia in Infants
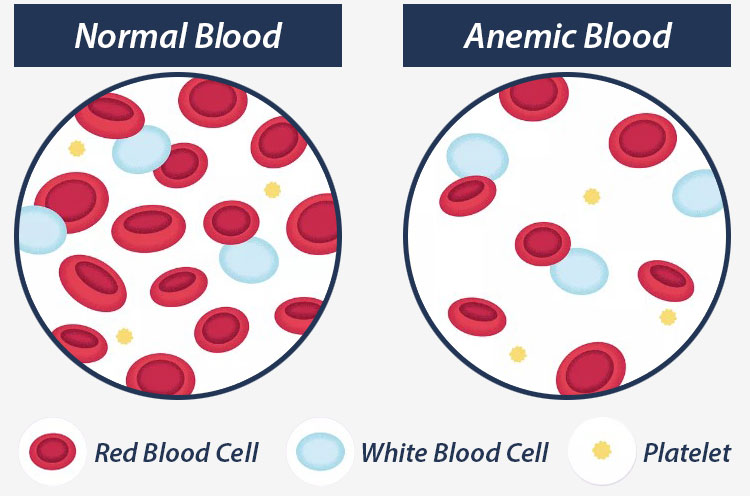
Anemia is a blood disorder where the blood lacks the typical number of red blood cells. Hemolytic anemia is a specific subtype where the body destroys red blood cells faster than it can replace them. If a baby develops hemolytic anemia, the excess bilirubin buildup from destroyed red blood cells can cause jaundice at birth.
Neonatal Infections
Neonatal infections can impact red blood cell production and impair the baby’s liver function. Maternal infections like group B strep, cytomegalovirus (CMV), or herpes simplex virus (HSV) sometimes transfer to the baby in utero. These infections can break down the baby’s red blood cells at an alarming rate and contribute to hyperbilirubinemia.
In addition, neonatal hepatitis infections directly weaken the baby’s liver, affecting its ability to process bilirubin. This can cause a buildup of unprocessed bilirubin, which can lead to newborn jaundice and a risk for kernicterus.
Neonatal Sepsis
Bacterial neonatal infections like group B strep, E. coli, or chorioamnionitis can trigger widespread inflammation in a newborns bloodstream. This inflammation, known as neonatal sepsis, can cause critical damage to the baby’s liver and red blood cell counts.
Neonatal sepsis is a life-threatening condition and a leading cause of infant mortality.
Issues with Breastfeeding

Breastfeeding assists with neonatal digestion and the newborn making their first bowel movements. Acting as a natural laxative, breast milk can help the baby expel excess amounts of bilirubin through their stool.
Newborns who have breastfeeding issues may experience dehydration and delayed bowel movements. When this occurs, their body reabsorbs the bilirubin that it would have otherwise excreted. The bilirubin returns back into the bloodstream and can build up to unsafe levels, causing jaundice and risks for kernicterus.
Medical professionals put babies at risk for complications when they miss these underlying causes of jaundice. If they misidentify the cause as harmless liver immaturity, they may delay critical intervention that could prevent kernicterus brain damage.
What Are Risk Factors for Jaundice & Kernicterus?

Certain characteristics of pregnancy or delivery can make a baby more likely to experience jaundice. These risk factors can include:
Premature Birth
Babies who arrive early (before 38 weeks gestation) have a higher risk for underdeveloped organs. If a premature baby’s liver is nonfunctional at the time of delivery, they have a higher risk for unprocessed bilirubin buildup.
Birth Trauma
Bruising or rupturing blood vessels during delivery can release a high volume of red blood cells. The baby may experience a surge in red blood cell production if they sustain injuries from a difficult delivery.
Common injuries can include cephalohematoma, bleeding from birth fractures, or injuries from misused delivery instruments like forceps and vacuum extractors.
Medications
Certain labor-inducing medications like Pitocin and Cytotec can increase a baby’s risk for developing jaundice after birth. Other antibiotics like nitrofurantoin and sulfonamides (synthetic antimicrobial medications) have links to increased bilirubin production in the newborn.
Maternal Infections
A mother’s infections during pregnancy like hepatitis, rubella, or syphilis can transfer to her baby through the placenta. This increases the baby’s risk of contracting neonatal infections that attack red blood cells and cause liver dysfunction.
Baby’s Medical Condition
Certain fetal complications can put a baby at higher risk for jaundice and kernicterus. Larger babies (macrosomia) experience increased red blood cell breakdown, which produces higher concentrations of bilirubin.
Also, conditions like fetal acidosis (acidic blood pH from oxygen deprivation) can damage the blood-brain barrier. This can allow unprocessed bilirubin to easily enter and cause kernicterus brain damage at birth.
Genetic Conditions
Additional factors like race, liver disorders, G6PD deficiency, and family medical history can increase a baby’s likelihood for jaundice. Medical professionals can sometimes spot signs of these underlying disorders during prenatal testing visits.
The medical professionals caring for a newborn should know when they have increased risks for hyperbilirubinemia, jaundice, or kernicterus. Early awareness of risk factors can allow for closer scrutiny, increased testing, and earlier treatment.
What Are Symptoms of Jaundice and Kernicterus?
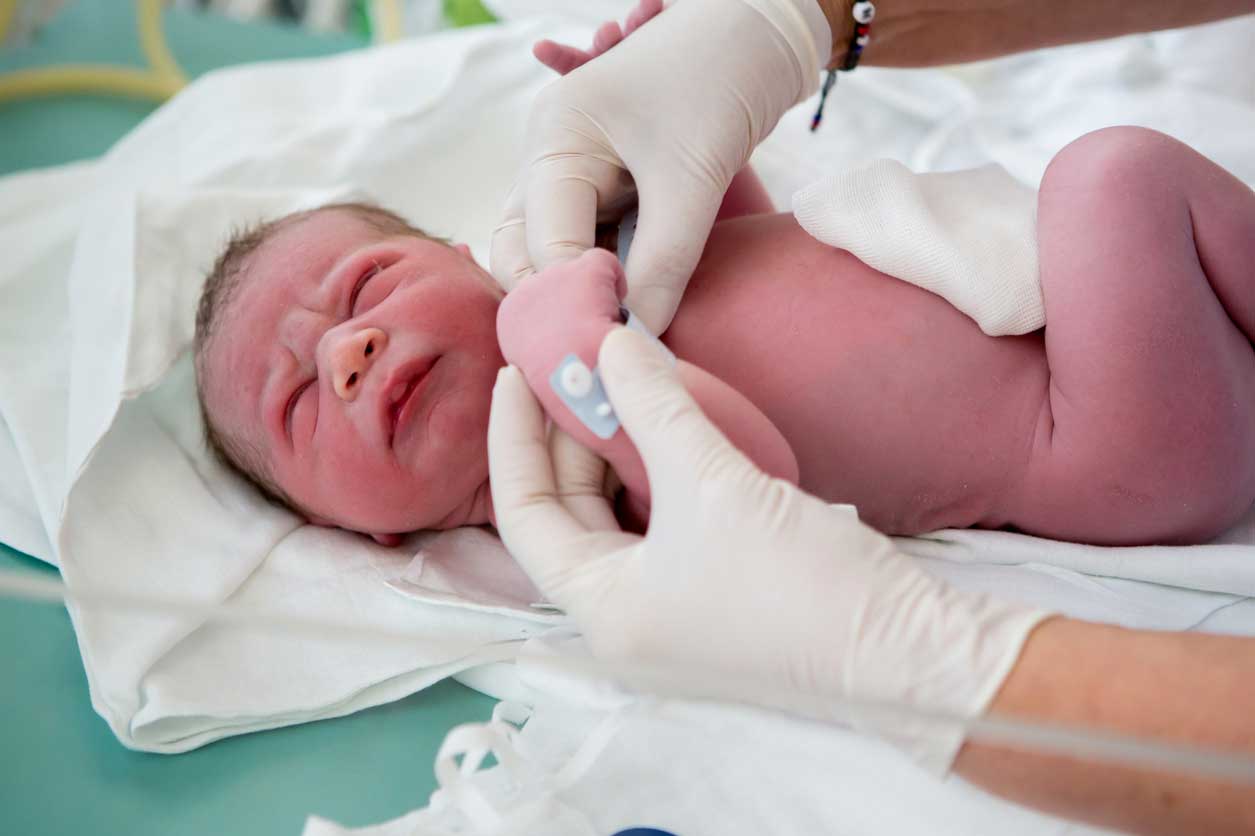
The key sign of jaundice is the yellow discoloration of the baby’s skin.
The yellow tint typically appears first on the newborn’s face before spreading to their chest, stomach, limbs, and eyes. It sometimes takes 2 to 3 days for the discoloration to begin.
Signs of Jaundice in Newborns
Other physical and behavioral signs of jaundice can include:
- Irritability: the baby is extremely fussy and inconsolable with a high-pitched cry
- Poor Feeding: the baby has a weak suck or other difficulties latching onto the mother’s breast for feeding
- Lethargy: the baby has difficulty staying awake or difficulty waking up for feeding
- Abnormal Stool or Meconium: the baby has infrequent bowel movements or no bowel movement at all. If they do, their stool may be pale and lightly colored (either beige or gray)
- Physical Weakness: the baby has delayed reflexes or appears overly floppy
- Other birth complications: conditions like acidemia or hypoglycemia frequently co-occur with jaundice symptoms
When a baby exhibits more than one of these symptoms alongside yellow skin, it usually indicates severe jaundice. Medical professionals must pay attention to these warnings to intervene before the baby develops kernicterus.
Signs of Kernicterus in Babies
Key signs of kernicterus brain damage can include:
- Extreme Discoloration: the baby’s skin discoloration reaches their eyes and/or takes on an orange/brown tint
- High Fever: the baby has a temperature reading that exceeds 100.4 degrees Fahrenheit
- Seizures: the baby begins convulsing with pauses in breathing
- Body Stiffness: the baby is rigid with extreme arching in the back
If a newborn shows any of these symptoms, it is a medical emergency. Medical professionals should immediately intervene to prevent further damage or infant death.
When a baby displays symptoms of jaundice, it’s crucial for healthcare workers to carefully monitor the situation. They should never assume the condition will resolve on its own. Failing to recognize the symptoms of severe jaundice or kernicterus can lead to permanent brain injuries and constitute medical malpractice.
How to Diagnose Jaundice in Newborns?
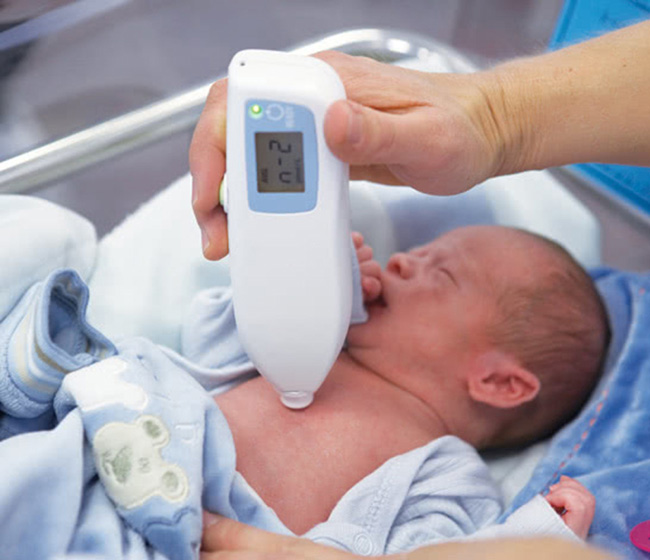
Diagnosing jaundice typically starts with a physical assessment of the newborn.
Doctors will examine the baby’s skin tone for a yellowish hue. If the baby has a darker skin pigment, the medical professional may press a finger down on their skin. This can reveal a yellowish pigment after they let off pressure on the skin.
But a visual assessment is often not enough to diagnose jaundice. Doctors and nurses will need to get a measurement of the baby’s bilirubin levels in their blood.
To do this, medical professionals may use a tool called a bilirubinometer. This is a non-invasive instrument that shines light on the baby’s skin to detect bilirubin levels. Bilirubinometers are highly accurate but may sometimes overestimate bilirubin levels in newborns with darker skin tones.
If medical professionals are not satisfied with the results, they may choose to move forward with blood testing. A total serum bilirubin test measures bilirubin concentrations from a sample of the baby’s venous blood (usually from their heel).
Other tests that help doctors diagnose jaundice include:
- Tests to check for Rh and ABO incompatibility
- Blood tests to check red blood cell counts
- Tests to measure liver function
What Should a Baby’s Bilirubin Level Be?
Doctors measure bilirubin in milligrams per deciliter of blood (or mg/dL, for short). A baby without jaundice will have bilirubin levels around 1-2 mg/dL at the time of birth. These levels will naturally rise and peak by day 3-4 of life at around 5-6 mg/dL.
A baby with physiological jaundice (non-concerning) will have bilirubin levels exceeding 5 mg/dL within the first 2 days of life. Around days 3-4, these levels can peak around 12 mg/dL. These are the cases that will normally resolve on their own.
But a baby’s bilirubin levels can be concerning when they exceed 15 mg/dL in the first 24-48 hours. This can indicate pathological jaundice, which stems from underlying causes and requires medical intervention. Key signs of neonatal pathological jaundice include high bilirubin levels from birth and/or bilirubin increases by over 5 mg/dL per day.
A baby’s risk for kernicterus becomes significant when their bilirubin levels exceed 25 mg/dL. Healthcare providers must carefully monitor the infant’s levels and intervene when appropriate to reduce the risk of permanent brain injuries.
What Are Treatments for Newborn Jaundice?

A baby’s medical team considers several factors when developing a treatment plan, including:
- Age
- Gestational age (how long the baby grew in its mother’s uterus)
- General health status and APGAR score
- Symptoms
- Type and severity of the baby’s jaundice (physiological jaundice vs pathological jaundice)
After medical professionals carefully assess the baby, they might begin one of the following treatments:
Phototherapy
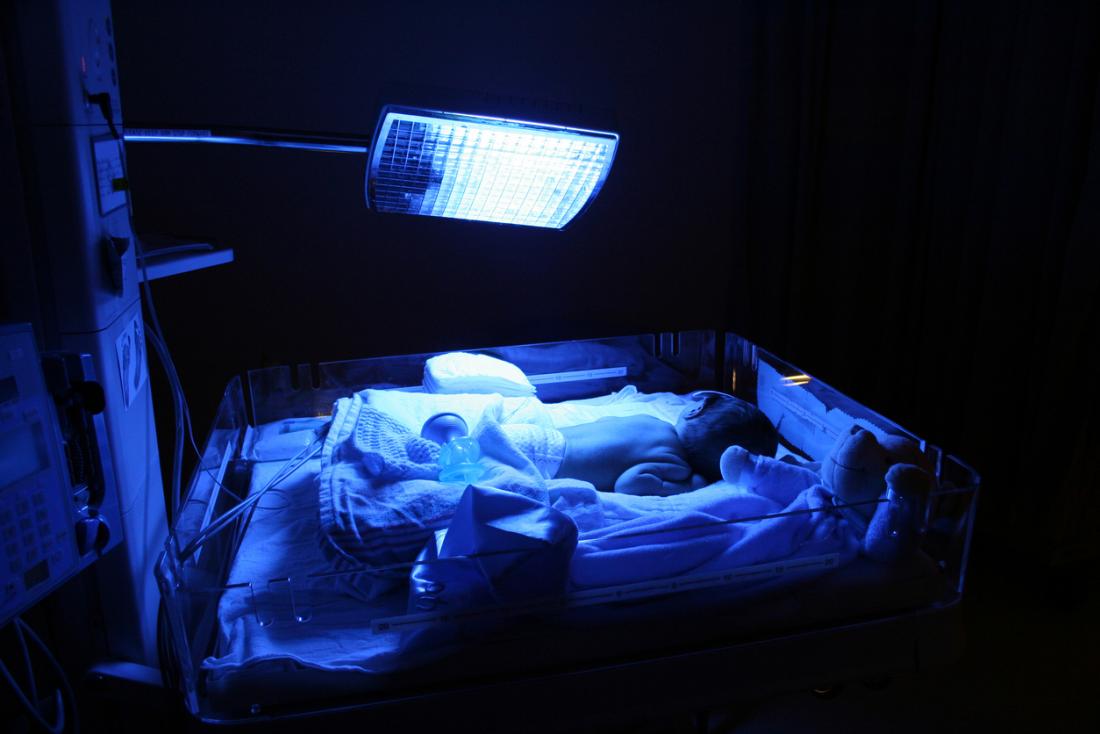
Phototherapy is a non-invasive treatment technique that places the baby under blue-green light for around 24 to 48 hours.
Because bilirubin absorbs light, placing the baby under special lights for a time can decrease high concentrations. Medical providers should cover the baby’s eyes to protect them from the lights. Also, staff members should carefully monitor the baby’s temperature throughout the process and test bilirubin levels every 4-12 hours.
Babies with a premature birth or especially high bilirubin levels may require longer treatment.
Fiber Optic Blankets
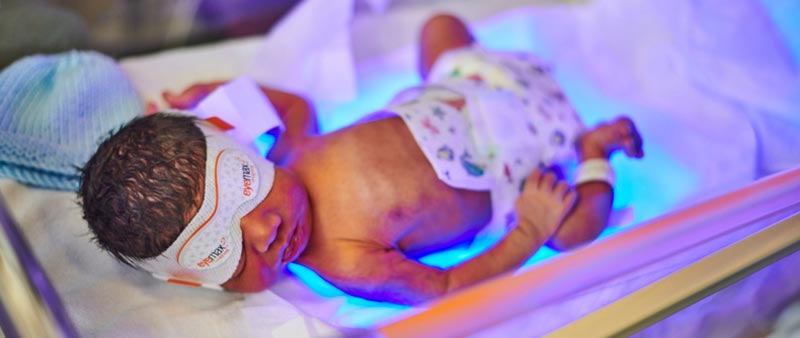
Like phototherapy, fiber optic blankets expose the baby to special lighting designed to decrease bilirubin levels. Healthcare providers place blankets containing fiber optic lights under the baby. Sometimes they will recommend combining phototherapy with fiber-optic blankets for maximum effect.
Exchange Transfusion
Exchange transfusion is an emergency procedure doctors may perform when the baby’s bilirubin levels are dangerously high. Doctors remove small amounts of the baby’s blood and replace it with blood containing less bilirubin.
Medical professionals will often consider exchange transfusion after phototherapy or fiber optic blankets fail to reduce bilirubin levels.
Supplemental Feedings
Sometimes breastfed babies develop jaundice because they are not getting enough milk. Doctors may recommend mothers supplement feedings with pumped breast milk or formula to prevent or reduce jaundice.
These treatment strategies can lower a newborn’s bilirubin levels back to normal and greatly reduce their risk for kernicterus. When the baby’s jaundice symptoms worsen over time or last over one week, doctors and nurses shouldn’t hesitate to intervene.
What Are the Complications of Jaundice?
Jaundice is highly treatable. Most babies with jaundice return to normal blood bilirubin levels within a few weeks.
But uncontrolled hyperbilirubinemia can cause bilirubin to cross the blood-brain barrier. When bilirubin enters the brain, severe, irreversible brain damage called kernicterus can occur.
Kernicterus damage is permanent, forever altering the lives of children and their parents. A child might need medication, therapies, surgeries, caregivers, and assistive technology to treat their resulting disabilities.
Medical Negligence Linked to Jaundice

Medical negligence and malpractice can sometimes be the root cause of birth injuries like kernicterus.
Specific examples of medical negligence when caring for newborns with jaundice include:
- Missing or ignoring the baby’s initial signs of jaundice like yellow skin
- Missing other jaundice symptoms like irritability, poor feeding, or lethargy
- Assuming a child’s jaundice is physiological and will clear up naturally
- Failing to test the baby’s bilirubin levels in the first 24 hours after birth
- Failing to regularly evaluate the baby’s bilirubin levels and missing large increases of over 5 mg/dL per day
- Misinterpreting the results of a bilirubinometer or a total serum bilirubin blood test
- Missing risk factors for jaundice like Rh and ABO incompatibility, neonatal infections, or fetal acidosis
- Injuring the baby during delivery, causing spikes in red blood cell production and increased bilirubin
- Failing to provide treatments for jaundice such as phototherapy or fiber optic blankets
- Missing the signs of kernicterus brain damage at birth
If you feel your child might be the victim of kernicterus malpractice, please contact our Jaundice Birth Injury Lawyers as soon as possible. We can investigate whether doctors or nurses committed any of the above errors in the days following your baby’s delivery.
Did Medical Negligence Cause My Child’s Brain Injury?

A child’s brain injury during birth can leave parents feeling scared, hopeless, and desperate for answers. They will want to know what caused the damage and if better medical care could have prevented it.
Our dedicated jaundice birth injury lawyers will help your family find those answers. We will evaluate all records during delivery and neonatal care to determine whether medical professionals properly diagnosed and treated jaundice.
If a family believes medical negligence worsened their child’s brain damage at birth, legal support may be an option. A specialized jaundice related birth injury attorney can review the medical records and circumstances to assess whether a claim exists.
Families who have experienced the effects of kernicterus from negligent medical care deserve to know whether they were avoidable. Our top rated birth injury lawyers will hold responsible parties accountable by pursuing birth injury malpractice claims.
What Is the Statute of Limitations in a Birth Injury Case?

A statute of limitations (SOL) is a law that sets a time limit on how long an injured person has to file a lawsuit after an accident.
It is essential to understand that statutes of limitations vary based on the case and the state where you file. For instance, the deadline for birth injury claims is typically different from other claims, such as injury to private property.
Generally, the clock starts ticking on the date the injury occurred. However, there are exceptions to this rule. In some cases, the statute of limitations starts when a person discovers or reasonably should have discovered an injury. When dealing with government agencies, SOLs can become even more complex.
For example, if the party that injured you was:
- A federal employee
- Employed by a military hospital, Veterans Administration facility, or a federally funded medical entity
You may need to file a birth injury claim under the Federal Tort Claims Act (FTCA). In FTCA cases, claimants must go through certain administrative procedures before filing a lawsuit. In some states, you may have less time to give notice if:
- The negligent party was a local or state government hospital
- The doctors and medical providers are employees of a governmental entity
If you file your case outside of the statute of limitations, the court will typically dismiss it. This means you will not be eligible to recover compensation for you or your child’s injuries.
Determining when a statute of limitations begins on your case can be tricky. Our jaundice birth injury lawyers can help inform you of all the important filing cutoff dates in your state. We will help your family seek justice and compensation for preventable injuries to you or your baby.
How Can Our Newborn Jaundice Attorneys Help?

Sometimes families are afraid to talk to lawyers about their child’s case. Others may simply feel overwhelmed by their circumstances and unable to participate in a lawsuit involving their child’s birth injury.
But the path toward justice always starts with speaking up. Finding the courage to contact a jaundice related birth injury lawyer could be the first step in securing compensation for your child. This compensation can help your family to afford care that will vastly improve your child’s quality of life, such as:
- Your child’s current and future medical treatment
- Caregivers or medical attendants
- Necessary assistive technology and equipment
- Physical therapy, speech therapy, or occupational therapy to restore independence
- Medications to treat related kernicterus complications like seizures or muscle spasms
Our Process
Our team of committed jaundice birth injury experts uses our detailed case review process to assess your potential claim. We start by learning more about you and your child. We will gather medical records to determine what happened before, during, and after your delivery. We call in skilled medical experts who review your records and let us know if they think medical errors could have caused your child’s injuries.
We will work to hold responsible parties accountable in a jaundice/kernicterus lawsuit case by pursuing birth injury malpractice claims against them.
At no point in our legal intake process will we ask you to pay anything. The medical review of your case and the consultation are free. We only receive payment once you do. The sooner you reach out, the sooner we can investigate your case and gather evidence to support your claim.
We work on a contingency fee basis, meaning you will not pay any legal fees until we win your case. We do not pursue any medical malpractice cases unless we fully believe we can win.
Contact us today to schedule your free consultation by calling our toll-free line at (888) 987-0005. You can also reach us by filling out our online request form.
National Birth Injury Law
Our National Birth Injury Attorneys, nurses, and support staff understand that parents of children with birth injuries feel overwhelmed. So, every client has the attention and support of a team of trained, compassionate professionals. But we don’t just offer compassion.
We offer a process to help you discover whether your child’s birth injury, HIE, cerebral palsy or brain injury at birth was caused by medical malpractice.
Call our offices today at (888) 987-0005 for experienced assistance in a free consultation.
Quick Links
Testimonials
- Lyric C. I feel like our voice was heard in a sense of what can possibly go wrong in a delivery and finding us answers. I feel with our settlement, we are now in a comfortable position to provide for our son.
- Lyssa L. They are not just people that say “hey let's get you money and let's go” The law firm was very thorough with us. It was awesome. I don't want to cry, because I think about and it's amazing that they were able to help me and that we were able to help my son and get the story out there.
- Jay C. Throughout the process, one thing was clear to us, the ultimate interest of our child was the utmost concern of Max and his team and as parents navigating a situation like that, that was refreshing to know we had them firmly on our side. I highly recommend them.
Popular Cities
- ★ Dallas Birth Injury
- ★ Houston Birth Injury
- ★ Atlanta Birth Injury
- ★ Chicago Birth Injury
- ★ Philadelphia Birth Injury
Locations
★ Dallas
11551 Forest Central Drive, Ste. 300
Dallas, TX 75243
★ Houston
12929 Gulf Freeway, Ste. 111
Houston, TX 77034