Amniotic Fluid Embolism
Amniotic Fluid Embolism During Labor and Delivery
An amniotic fluid embolism (AFE) is a life-threatening medical emergency that requires an immediate response from specialized healthcare teams. Symptoms can appear with little warning and escalate rapidly, threatening the wellbeing of a mother and her child during labor.
Much about amniotic fluid embolisms remain unknown; researchers haven’t been able to define a definite cause or explain why it occurs some women and not others. For this reason, an AFE can be difficult to predict.
However, medical negligence and medical malpractice can occur when treating women suffering from an AFE. Incorrect treatment steps or failing to act with the appropriate urgency can cause further harm to the mother and/or her baby, lowering their odds of survival and potentially leaving them with long-lasting birth complications.
A newborn can sustain a devastating birth injury without proper treatment during and after an amniotic fluid embolism. Miller Weisbrod Olesky has a decades-long track record of results for children and families across the United States who have suffered from all types of improperly-treated labor and delivery complications. Our experienced team of birth injury attorneys can review the unique circumstances of you or your family’s case to deliver the treatment, care, and financial resources you deserve.
Free Legal Consultation
Birth Injury Lawyers
(888) 987-0005Our Birth Injury Lawyers are available to meet you in your home or the hospital.
What is an Amniotic Fluid Embolism?
Amniotic fluid is a liquid within the uterus that surrounds the fetus during pregnancy. It is crucial to temperature regulation, organ development, and fetal protection from impacts while the child grows in the womb.
A mother’s contractions and the natural separation of the placenta from her uterine lining place stress on her womb during labor. This creates small uterine and cervical microtears, exposing open blood vessels for amniotic fluid to travel. This is a common and natural experience for most women during labor. Amniotic fluid (as well as other fetal material such as cells and hair) typically enters the bloodstream in very small amounts with no consequence to the mother’s overall health.

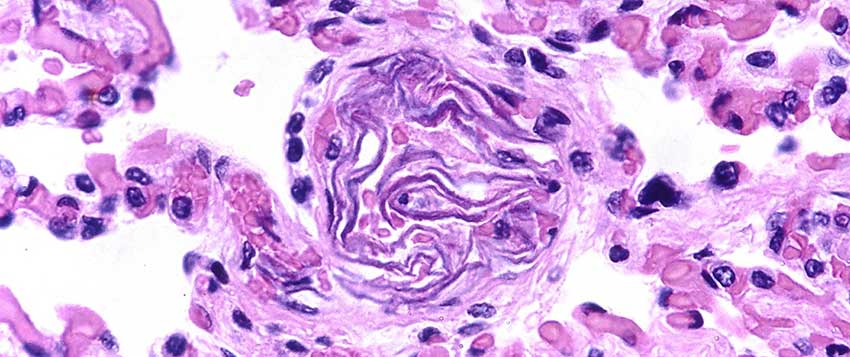
However, some women in rare cases develop an allergic-like reaction; their body’s immune system registers the fluid as an external threat and triggers an inflammatory response. The inflammation causes blood clotting in blood vessels that can travel through the bloodstream to the lungs, which results in an amniotic fluid embolism. It is also sometimes referred to as anaphylactoid syndrome of pregnancy (ASP).
Amniotic fluid embolisms are rare but deadly. They are estimated to occur in 1 in 40,000 deliveries in the United States, and the maternal mortality estimates vary from 20-60%. The variance in death rates is due to the ambiguity regarding whether the cause of death was the AFE or a related labor complication.
What Are the Symptoms for an Amniotic Fluid Embolism?
Symptoms of an AFE can appear without warning and progress rapidly in severity. The signs typically are broken into two phases:
- Phase One (Rapid Respiratory Failure): Symptoms include cardiopulmonary collapse, cardiac arrest, blood clotting, shortness of breath, hypoxia (oxygen loss for the mother and potentially the child, depending on the stage of labor), pulmonary hypertension, and a sudden drop in blood pressure. The mother may also experience nausea, vomiting, and seizures. This is the phase of an Amniotic Fluid Embolism with the highest fatality rates, so immediate treatment of these symptoms is critical.
- Phase Two (Hemorrhaging): In this phase (typically right after giving birth), symptoms include uncontrollable bleeding from the mother’s uterus where the placenta was detached. If the AFE forced her to have an emergency c-section, she may have hemorrhaging near the incision area as well. Excessive internal bleeding can expose the mother to a number of serious health risks, including organ failure and infection.
What are the Common Complications Caused by AFE?
An amniotic fluid embolism can be life-threatening for the mother, which consequently puts her child at an increased risk for the following severe birth injuries:
Hypoxic Brain Injuries
Depending on the stage of labor in which the AFE occurred, it’s possible for the baby’s oxygen supply to get cut off prematurely, making them vulnerable to various hypoxic (lack of oxygen) and ischemic (lack of blood flow) brain injuries like Hypoxic-Ischemic Encephalopathy (HIE) and cerebral palsy. These brain injuries come with long-lasting birth complications to the child’s physical and cognitive health, including varying levels of paralysis and developmental delays.
Fetal Distress and Fetal Bradycardia
Research suggests that for some cases of AFE, fetal distress was first identified in the child before any maternal symptoms became present. Doctors usually use fetal heart rate monitoring to identify when a baby is in fetal distress, and it is typically characterized by a lack of oxygen and abnormally slow heart rates (bradycardia).
Fetal bradycardia that is not diagnosed or corrected well in time may lead to serious long-term effects for the baby. The fetal or neonatal outcomes may include nerve damage, brain damage, hypoxia or anoxia, paralysis, cerebral palsy, and in some instances even death.
It is critical that all babies be monitored during the labor and delivery process with electronic fetal monitoring equipment to detect whether or not bradycardia is occurring. When the cause of fetal bradycardia cannot be determined or reversed or it persists, immediate delivery is usually recommended including by emergency c-section.
Risk of Miscarriage or Fetal Death
A 2016 study suggests approximately 30% of infants do not survive complications from an AFE. However, an infant’s survival rate will heavily depend on the stage of labor the mother has progressed to. If the expectant mother is still in the beginning of labor when she develops an embolism, the baby’s chances of survival are lower.
What Causes Amniotic Fluid Embolisms?
Even though the first case of Amniotic Fluid Embolism was discovered in 1926, researchers still do not know why amniotic fluid in the bloodstream affects some women and not others. For this reason, there currently isn’t any known preventative measures women can take to guarantee she won’t have an amniotic fluid embolism. However, certain risk factors exist that may increase a woman’s risk for an amniotic fluid embolism.
What Are Risk Factors for Amniotic Fluid Embolisms?
If a mother’s body does reject amniotic fluid, there are several risk factors that will increase her likelihood of developing an embolism. They include:
- A higher-than-average maternal age (pregnancy at age 35 and older)
- Expecting multiples (pregnancy with twins or triplets)
- An amniotic fluid complication such as polyhydramnios (too much amniotic fluid) or oligohydramnios (too little amniotic fluid)
- Placental issues like placenta previa or a placental abruption
- Preexisting uterine or cervical tears
- A preeclampsia or eclampsia diagnosis
- Taking certain labor induction medications
How to Diagnose an Amniotic Fluid Embolism?
Doctors and other professional healthcare providers must be aware of the signs and symptoms of an amniotic fluid embolism. Sometimes, the symptoms of an AFE can be indicative of a different labor and delivery complication, making it tricky to know for sure. But healthcare specialists must evaluate all of the mother’s symptoms and use their judgement to determine her status, because quick treatment is imperative to her and her child’s survival.
Healthcare professionals may be able to use the following signs to diagnose an amniotic fluid embolism:
- Prolonged blood clotting times in blood test results
- The mother has low oxygen levels
- The mother has difficulties with breathing
- Fluid is detected in the patient’s lungs (pulmonary edema)
- The mother has an abnormally high heart rate (tachycardia)
- The mother is bleeding profusely from the uterus
- The mother is exhibiting agitation or sudden confusion (or other early signs of a stroke)
Can Medical Negligence Cause an Amniotic Fluid Embolism?
Amniotic fluid embolisms can be unpredictable and nearly impossible to prevent. However, there are different treatments and aftercare procedures that healthcare specialists are expected to follow to ensure the mother and her child do not suffer a serious birth injury. If an AFE occurs, there may be medical negligence or even medical malpractice if the labor and delivery medical team fails to carry out any of the following actions:
- Failure to carry out an emergency c-section delivery in time, resulting in the child’s death or a severe birth injury.
- Failure to conduct necessary diagnostic tests after an AFE, such as an electrocardiogram (EKG), echocardiogram, or chest x-rays.
- Failure to use a pulse oximeter to monitor the mother’s blood oxygen levels.
- Failure to recognize fetal distress via improper fetal heart rate monitoring.
- Making errors or skipping steps while operating on a mother or her child during an AFE.
- Improper neonatal care following a child’s birth after a mother’s AFE.
Were My or My Child’s Amniotic Fluid Embolism Injuries Preventable?
Injuries sustained from an amniotic fluid embolism can sometimes be prevented with the proper medical treatment. If someone believes medical negligence contributed to their child’s birth injury, legal support may be an option. A knowledgeable birth injury attorney can review the medical records and circumstances to assess whether a claim exists.

Parents whose children suffer from related birth complications of an amniotic fluid embolism, as well as parents who have suffered the loss of their baby, deserve to know whether the complications resulting from it were preventable. Our dedicated birth injury lawyers want to help you find those answers and obtain the funds necessary to purchase devices that can help improve the quality of your child's life.
If your child has been diagnosed with a birth injury after a medical procedure and you suspect it may have been caused in part by medical mistakes, Miller Weisbrod Olesky will thoroughly investigate the facts and hold responsible medical providers accountable by pursuing medical malpractice claims against them.
Sometimes families are hesitant to reach out to a medical malpractice attorney or law firm. Parents may feel overwhelmed by their circumstances or are worried that a law firm will not be able to help them. But the only way to find out if you have a case is to talk to an attorney who understands how birth injuries can lead to developmental delays and other complications that require long-lasting medical support.
How Long Do I Have to File an Amniotic Fluid Embolism Related Lawsuit?

A statute of limitations (SOL) is a law that sets a time limit on how long an injured person has to file a lawsuit after an accident. It is essential to understand that statutes of limitations vary based on the type of case and the state where it is filed. For instance, the deadline for birth injury claims is typically different from other claims, such as injury to personal property, fraud, contract disputes, and collection of debts.
Generally, the clock starts ticking on the date the injury occurred. However, there are exceptions to this rule, and in some cases, the statute of limitations starts when a person discovers or reasonably should have discovered an injury. When dealing with government agencies, SOLs can become even more complex.
For example, if the party that injured you was:
- A federal employee
- Employed by a military hospital, Veterans Administration facility, or a federally funded medical entity
You may need to file a birth injury claim under the Federal Tort Claims Act (FTCA). In FTCA cases, claimants must go through certain administrative procedures before filing a lawsuit. In some states, if the negligent party was a local or state government hospital or the doctors and medical providers are employees of a governmental entity, the time period in which you must give "notice" may be shorter.
If your case is filed outside of the statute of limitations, it will typically be dismissed, and you will not be eligible to recover compensation for your injuries. Determining when a statute of limitations begins on your case can be tricky. If you're considering pursuing compensation for a birth injury, contacting an attorney as soon as possible is in your best interest.
How The Birth Injury Attorneys at Miller Weisbrod Olesky Can Help?
 It takes a detailed expert review of the facts and circumstances of your child's birth to determine whether the complications from an amniotic fluid embolism stemmed from medical malpractice.
It takes a detailed expert review of the facts and circumstances of your child's birth to determine whether the complications from an amniotic fluid embolism stemmed from medical malpractice.
At Miller Weisbrod Olesky, a team of committed birth injury attorneys, nurses and paraprofessionals uses our detailed medical negligence case review process to assess your potential birth injury case. We start by learning more about you and your child and the status of delayed/missing developmental milestones. Then we gather medical records to determine what happened before, during, and after your delivery. We call in skilled medical experts who review your records and let us know if they think medical errors could have caused your child's injuries.
If we feel medical negligence caused or contributed to your child's injuries, we meet with you to discuss how you can receive compensation from the medical professionals who made the errors.
At no point in our legal intake process will we ask you to pay anything. The medical review of your case and the consultation are free. We only receive payment when you do. The sooner you reach out to us, the sooner we can begin investigating your case and gathering the evidence needed to support your claim.
We work on a contingency fee basis, meaning you won't pay any legal fees unless we win your case. Contact us today to schedule your free consultation by calling our toll-free line at (888) 987-0005 or by filling out our online request form.
Contact Miller Weisbrod Olesky
National Birth Injury Law
Our National Birth Injury Attorneys, nurses, and support staff understand that parents of children with birth injuries feel overwhelmed. So, every client has the attention and support of a team of trained, compassionate professionals. But we don’t just offer compassion.
We offer a process to help you discover whether your child’s birth injury, HIE, cerebral palsy or brain injury at birth was caused by medical malpractice.
Call our offices today at (888) 987-0005 for experienced assistance in a free consultation.
Quick Links
Testimonials
- Lyric C. I feel like our voice was heard in a sense of what can possibly go wrong in a delivery and finding us answers. I feel with our settlement, we are now in a comfortable position to provide for our son.
- Lyssa L. They are not just people that say “hey let's get you money and let's go” The law firm was very thorough with us. It was awesome. I don't want to cry, because I think about and it's amazing that they were able to help me and that we were able to help my son and get the story out there.
- Jay C. Throughout the process, one thing was clear to us, the ultimate interest of our child was the utmost concern of Max and his team and as parents navigating a situation like that, that was refreshing to know we had them firmly on our side. I highly recommend them.
Popular Cities
- ★ Dallas Birth Injury
- ★ Houston Birth Injury
- ★ Atlanta Birth Injury
- ★ Chicago Birth Injury
- ★ Philadelphia Birth Injury
Locations
★ Dallas
11551 Forest Central Drive, Ste. 300
Dallas, TX 75243
★ Houston
12929 Gulf Freeway, Ste. 111
Houston, TX 77034