Group B Strep
Group B Strep During Pregnancy
Adverse neonatal outcomes sometimes result from maternal infections, including intrauterine, cervical, vaginal, or in rare cases, non-pelvic infections. The most common maternal infection linked to injuries for the baby is Group B Streptococcus (Group B Strep or GBS).
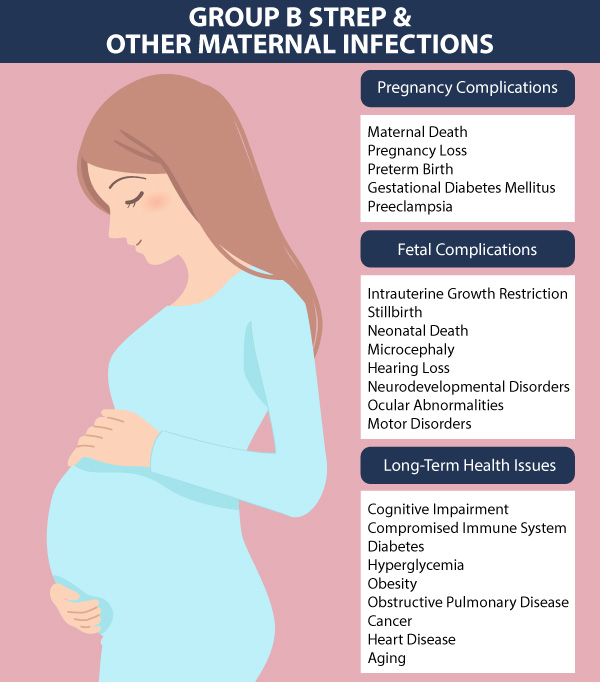
Maternal infections like Group B Streptococcus can cause birth complications like neonatal infection or a premature birth. These complications can serve as an underlying cause of birth injuries, resulting in long-term neurologic or brain damage at birth. Neonatal brain injuries like hypoxic ischemic encephalopathy (HIE) commonly lead to a cerebral palsy diagnosis later in childhood.
OB-GYNs, nurses, and all other medical professionals must thoroughly screen expecting mothers for Group B Strep during prenatal testing appointments. The infection is easily treatable with antibiotic medications, but treatment is most effective when healthcare professionals start it early.
Failing to catch or properly treat Group B Strep infections increases the mother’s risk of passing it to her baby. This can lead to preventable birth defects and birth injuries and constitute medical malpractice.
Birth Injury Malpractice Attorneys
Our top rated birth injury attorneys specialize in identifying how medical errors lead to severe birth injuries. If you or someone you know suffered from injuries after a mismanaged maternal infection, don’t hesitate to contact our firm. We can answer difficult legal and medical questions and investigate the facts on your behalf.
Free Legal Consultation
Birth Injury Lawyers
(888) 987-0005Our Birth Injury Lawyers are available to meet you in your home or the hospital.
Our vast network of medical experts and in-house nursing staff and nurse-attorneys gives us the edge over our competition. When we take your case, we assign you with an entire medical team. This team not only consists of attorneys but also nursing advocates and medical experts.
Your team is available to assist with any day-to-day treatment you or your child may need. This includes assistance with medical records, scheduling doctors’ appointments, providing transportation, and any other problems that may arise.
We offer all of this on a contingency fee basis. This means you will not pay any fees until after we win your case and secure a settlement. Miller Weisbrod Olesky’s unmatched track record of birth injury results sets us apart from other birth injury law firms.

Recent Birth Injury Settlement:
Birth Injury settlement against a hospital in which nurses and physicians failed to properly monitor the mother's blood pressure during delivery causing an HIE event resulting in neonatal seizures and cerebral palsy at birth. Our team of top-rated birth injury lawyers recovered $13,750,000 for the family to help with future medical expenses and developmental therapy.
What is Group B Strep?
Group B Streptococcus is a common bacterial infection occurring in either the genitourinary (genital and urinary) or gastrointestinal (digestive) tract. About one in four expecting mothers contract the infection, and most of these women have asymptomatic cases.
Group B Strep (GBS) is the most common and preventable infection that expecting mothers contract and transmit to their babies. Babies who catch the infection and don’t receive immediate and aggressive treatment are at high risk for birth injuries.
★ Genitourinary Tract: beginning at the kidneys. A retroperitoneal organ located at T12-L3 whose primary function is to filter blood and secrete waste products as urine.
★ Gastrointestinal Tract: lso called digestive tract or alimentary canal. The pathway where food enters the body and solid wastes exit. The gastrointestinal tract includes the mouth, pharynx, esophagus, stomach, small intestine, large intestine, and anus.
In the U.S., doctors recognize GBS as the most common maternal infection causing invasive GBS (iGBS) disease in babies. Neonatal iGBS diseases include sepsis (blood infection) and meningitis (inflammation of the brain and spinal cord tissue).
Adverse outcomes of iGBS in babies include preterm birth, stillbirth, and neurodevelopmental impairment (NDI). Neurodevelopmental impairment includes hearing difficulties, vision impairments, cognitive impairment, or cerebral palsy symptoms.
How does Group B Strep Infect the Baby?
An expecting mother infected with GBS can transmit the infection to her baby during vaginal delivery. The primary route of GBS in babies is vertical transmission during passage from the vagina during labor & delivery. The onset of GBS in babies may occur as follows:
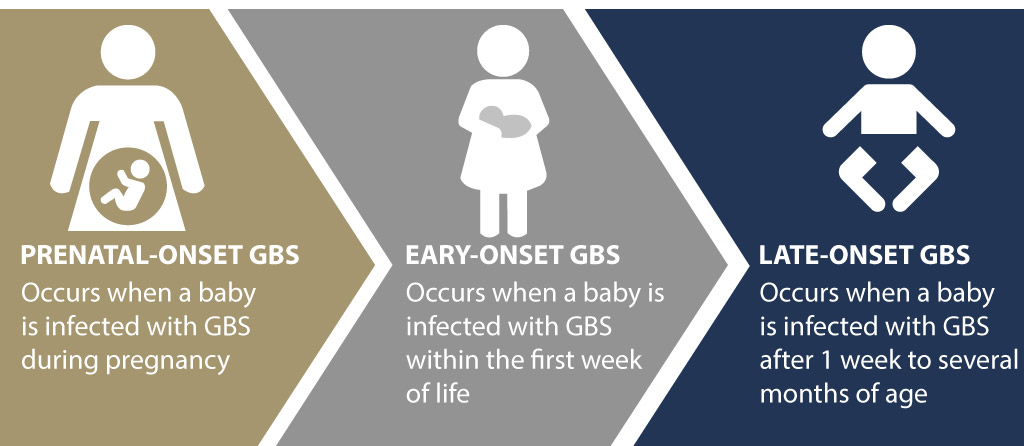
- Early Onset iGBS (EOGBS) infection: In about 75% of all babies with GBS, the neonatal infection may present in 0 to 6 days after birth. Colonization of the Group B Strep bacteria in the maternal genitourinary track is most common with early onset cases.
- Late Onset iGBS (LOGBS) infection: This form of GBS infection is less common in babies but may present within 7 to 89 days after birth. These babies are at a risk of developing neurodevelopmental impairments (NDI) or cerebral palsy.
What Risk Factors Exist for Group B Strep Infection?

The CDC recommends prenatal screening for all expecting mothers for GBS during the 35 to 37 weeks gestation of pregnancy. This means that GBS screening is the “standard of care” for obstetricians and other medical professionals caring for the mother.
GBS testing involves obtaining a swab of the vaginal and rectal areas. The healthcare provider then sends the swab to a laboratory for analysis.
If the GBS culture test returns as positive, her medical team should consider it a marker of heavy bacterial colonization. This means the baby is at considerable risk for contracting the infection if doctors do not take appropriate action.
Medical providers should also consider additional risk factors for early onset GBS, such as:
- Young maternal age
- Preterm labor (under 37 weeks)
- Maternal fever above 100.4 F during labor
- Premature rupture of membranes (PROM)
- History of a previous child with invasive early onset GBS neonatal infection
- Being of Hispanic or African American descent
- Maternal Obesity
- Gestational Diabetes
According to researchers, early onset iGBS may infect about 2% of the babies born to mothers with GBS.
Diagnosing Group B Strep During Pregnancy

Expecting mothers with GBS will typically be asymptomatic, which makes it critical to always test in the third trimester. Lab-tested culture swab samples are the easiest way to determine if the mother is GBS “positive.” It can take two to three days to obtain the results because the GBS bacteria need time to grow (culture).
In some cases, Group B Strep bacteria can cause urinary tract infections (UTIs). Doctors can diagnose UTIs by testing a sample of the mother’s urine.
Symptoms in an expecting mother can include:
- Frequent urination or urge to urinate
- Pain during urination
- Vomiting and nausea
- Fever
- Pain in the back or side
- Soreness in the belly
- Increased heart rate
Diagnosing Group B Strep After Birth

Babies with early onset invasive GBS may display some or all of the following signs and symptoms:
During the first 24 hours after birth
- Lethargic, sleepy, fussy, and having signs of respiratory distress (as well as signs of sepsis)
- Breathing difficulties with long periods without breathing (signs of meningitis)
- Rapid breathing with grunting sounds (signs of pneumonia)
- Fluctuations in blood pressure levels
- Experiencing seizures (convulsions)
During the first week after birth
- Reduced movement in a leg or arm
- Painful movement in a leg or arm
- Fever
- Breathing difficulties
- Redness in a part of the face or other body parts
If doctors suspect GBS in a baby after birth, the medical provider should obtain blood samples to test. If the baby shows signs of sickness, the doctor may perform additional tests such as urine cultures or chest x-rays.
How to Treat and Manage Neonatal GBS?

Once doctors suspect the baby to have a group B strep infection, they must receive immediate support and antibiotic administration.
The treatment must happen initially within the age-appropriate critical care setting. The gold standard is that no more than an hour passes between deciding to treat the baby and administering antibiotics. This must occur even if the culture results have not come back from the lab to prevent serious complications.
In case of early onset sepsis, doctors generally prescribe amoxycillin/ampicillin (with a broader spectrum than penicillin). If the baby has meningitis, doctors generally recommend cefotaxime or another cephalosporin medication because of its more optimal tissue penetration.
How to Prevent Neonatal Group B Strep Transmission?

A universal GBS culture-based screening between weeks 36 and 37 of gestation is the standard of care. However, another marker of infection in the genital tract is GBS bacteriuria (infection of the amniotic fluid, placenta, or membranes.)
All expecting mothers should undergo screening for asymptomatic bacteriuria. When tests detect GBS bacteriuria at any stage of the pregnancy, doctors should quickly administer preventative antibiotic medications.
The principal clinical defense against the risk of early onset of iGBS infection is timely administration of prophylaxis (preventative) antibiotics. Medical providers should also assess cases where mothers would more likely benefit from antibiotic administration during labor and delivery.
Expecting mothers will typically receive antibiotics for GBS intravenously (through the vein). One of the most common antibiotics are beta-lactams, which contain penicillin and ampicillin. If the woman has an allergy to these antibiotics, the OB-GYN or maternal fetal medicine specialist must prescribe other antibiotics. Preventative antibiotics are the most critical measure to avoid the transmission of the GBS infection to the baby.
About 10% of mothers will experience mild side effects after taking penicillin. Severe allergic reactions are rare (observed in about 1 in 10,000 women), which makes the antibiotics treatment generally very safe. Doctors must always take note of a mother’s medical history before prescribing any type of medication.
During pregnancy and labor, the efforts to prevent GBS infection transmission to the baby should be a coordinated team effort. The team caring for the expecting mother should diligently screen her for GBS. This medical team may include physicians like obstetricians or maternal fetal medicine specialists, physician assistants, nurse practitioners, nurses, and/or midwives.
Even if there is no positive GBS culture, doctors should administer preventative antibiotic treatment to:
- Expecting mothers who are delivering their baby prior to the 37th week of their pregnancy and have a low-grade temperature.
- Expecting mothers in a prolonged labor who have not delivered for more than 18 hours after their water breaks.
- Expecting mothers who have delivered a previous baby with a GBS neonatal infection.
Was My Group B Strep Infection Missed or Mismanaged During Pregnancy?

Medical professionals must screen for many common maternal infections such as Group B Strep during prenatal testing. Medical negligence can worsen a mother’s health and expose their vulnerable baby to dangerous neonatal infections. Examples of negligent acts include misdiagnoses, failure to catch early symptoms of GBS, or failing to administer sufficient antibiotic treatment.
If a family believes medical negligence contributed to a child’s neonatal infection, legal support may be an option. A specialized birth injury attorney can review the medical records and circumstances to assess whether a claim exists.
Families who have experienced the effects of birth injuries deserve to know whether better medical care could have prevented them. Our top rated birth injury lawyers will help you find those answers and obtain the necessary funds to secure treatment.
Our team at Miller Weisbrod Olesky will thoroughly investigate the facts, holding responsible parties accountable by pursuing medical malpractice claims.
What is the Statute of Limitations in a Birth Injury Lawsuit?

A statute of limitations (SOL) is a law that sets a time limit on how long an injured person has to file a lawsuit after an accident. It is essential to understand that statutes of limitations vary based on the case and the state where you file. For instance, the deadline for birth injury claims is typically different from other claims, such as injury to private property.
Generally, the clock starts ticking on the date the injury occurred. However, there are exceptions to this rule. In some cases, the statute of limitations starts when a person discovers or reasonably should have discovered an injury. When dealing with government agencies, SOLs can become even more complex.
For example, if the party that injured you was:
- A federal employee
- Employed by a military hospital, Veterans Administration facility, or a federally funded medical entity
You may need to file a birth injury claim under the Federal Tort Claims Act (FTCA). In FTCA cases, claimants must go through certain administrative procedures before filing a lawsuit. In some states, you may have less time to give notice if:
- The negligent party was a local or state government hospital.
- The doctors and medical providers are employees of a governmental entity.
If you file your case outside of the statute of limitations, the court will typically dismiss it. This means you will not be eligible to recover compensation for you or your child’s injuries. Determining when a statute of limitations begins on your case can be tricky. If you are considering pursuing compensation for a birth injury, contact an attorney as soon as possible.
How Can Our Birth Injury Attorneys Help?

Maternal infections and neonatal infections can cause injuries and complications for both an expecting mother and her child. It takes an expert review of the facts of your birth to determine whether medical professionals made preventable errors.
Our Process
Our team of committed attorneys, nurses and paraprofessionals works to answer these questions and seek compensation. We use our detailed medical negligence case review process to assess your potential birth injury case.
We start by learning more about your child by gathering records to determine what happened during and after their birth. This includes a detailed review of the treatment doctors provided or failed to provide during prenatal testing appointments.
We will call in skilled medical experts who review your records and provide insight into where medical professionals went wrong. If we feel medical negligence caused or worsened your child’s injuries, we meet with you to discuss further.
At no point in our legal intake process will we ask you to pay anything. The medical review of your case and the consultation are free. We only receive payment once you do. The sooner you reach out, the sooner we can investigate your case and gather the evidence to support your claim.
We work on a contingency fee basis, meaning you will not pay any legal fees until we win your case. We do not purse any medical malpractice cases unless we fully believe we can win. Contact us today to schedule your free consultation by calling our toll-free line at (888) 987-0005. You can also reach us by filling out our online request form.
Contact Our National Birth Injury Lawyers
National Birth Injury Law
Our National Birth Injury Attorneys, nurses, and support staff understand that parents of children with birth injuries feel overwhelmed. So, every client has the attention and support of a team of trained, compassionate professionals. But we don’t just offer compassion.
We offer a process to help you discover whether your child’s birth injury, HIE, cerebral palsy or brain injury at birth was caused by medical malpractice.
Call our offices today at (888) 987-0005 for experienced assistance in a free consultation.
Quick Links
Testimonials
- Lyric C. I feel like our voice was heard in a sense of what can possibly go wrong in a delivery and finding us answers. I feel with our settlement, we are now in a comfortable position to provide for our son.
- Lyssa L. They are not just people that say “hey let's get you money and let's go” The law firm was very thorough with us. It was awesome. I don't want to cry, because I think about and it's amazing that they were able to help me and that we were able to help my son and get the story out there.
- Jay C. Throughout the process, one thing was clear to us, the ultimate interest of our child was the utmost concern of Max and his team and as parents navigating a situation like that, that was refreshing to know we had them firmly on our side. I highly recommend them.
Popular Cities
- ★ Dallas Birth Injury
- ★ Houston Birth Injury
- ★ Atlanta Birth Injury
- ★ Chicago Birth Injury
- ★ Philadelphia Birth Injury
Locations
★ Dallas
11551 Forest Central Drive, Ste. 300
Dallas, TX 75243
★ Houston
12929 Gulf Freeway, Ste. 111
Houston, TX 77034